A new trial shows that we can accelerate orthodontic tooth movement!
A new trial shows that we can accelerate orthodontic tooth movement!
I have posted before about the various new methods of attempting to accelerate orthodontic tooth movement. Most of these studies were inconclusive, poorly done or revealed that the new developments were not effective. But, we now have a trial that shows that orthodontic tooth movement can be accelerated.
C. Charavet et al
Journal of Dental Research 2016, Vol. 95(9) 1003–1009 DOI: 10.1177/0022034516645066
This research was carried out by a team based in Liege, Belgium. It was published in the Journal of Dental Research, which is a really hard journal to get into.
They outlined that one new approach to accelerate tooth movement is piezocision. This is a localised piezoelectric alveolar decortication that combines buccal micro incisions and minimally invasive corticotomies that are performed with a piezotome.
The aim of their randomised trial was;
“to determine the efficacy of piezocision-acclerated orthodontic treatment”.
The primary outcome measure was duration of treatment in months.
Secondary outcomes were periodontal health, alveolar crest changes, bone and gingival healing and analgesic intake.
Their sample size calculation showed that they needed 10 patients per group to detect a difference in 20% of treatment duration.
They included 24 adult patients with minimal to moderate anterior crowding, who required upper and lower fixed appliance treatment.
The patients were randomised using sealed envelope concealment with a pre-prepared blocked randomisation. They were allocated to receive piezocision or control treatment as usual. All the patients were treated with Damon brackets but I was not clear on whether this was done by one operator. The patients attended the clinic every two weeks to have their appliances adjusted.
The end of treatment was defined as
- Class I
- Complete correction of upper and lower maxillary and mandibular crowding
- Optimal overjet and overbite (from 1 to 2 mm)
What did they find?
12 patients were allocated to receive piezocision and 12 were in the control group. They all completed the study.
They found that the overall treatment time was less for the piezocision group than the control. There were also shorter times for the period between arch wire changes. They presented the data as box plots and I could not find the mean treatment times for each group anywhere in the paper. From the box plots I estimated that the median treatment time was 310 days for the piezocision group and 550 days for the control group. They stated that this represented a 43% reduction.
There were no major harms from having the procedure and the patients were happy with the treatment.
They felt that results of their trial should be interpreted with some caution because the malocclusions were very mild and confined to crowding.
Their overall conclusion was
“Based on these results, piezocision can be considered a promising new therapeutic tool for orthodontic treatment”.
We need to note that these are cautious conclusions, as they stated the technique is promising.
What did I think?
This was a good small study that came to a clear conclusion. The study was well carried out and written well. I agree with the authors that the study results need to be interpreted with a degree of conclusion for the following reasons:
- The malocclusions were mild and this intervention needs testing on more severe problems.
- The patients were seen at rather short intervals
- The sample size was small and while this satisfied the sample size calculation the results are subject to individual variation.
- The data was not clearly presented and I would have liked to see the values in a table with 95% confidence intervals.
- It was not clear if there were more than one operator in the study and this may have had an effect on the results. I may have missed this in the paper and perhaps the authors could answer this question.
Overall, this was an interesting study that came to a clinically useful conclusion. This technique should be evaluated in further trials, as it may have potential to modify our practice. I also wonder if this is a little too invasive for most patients and orthodontists, but they reported that the patients did not have many complaints. In reality, there is probably a “trade off” between some discomfort and a reduce treatment time.
There may be something to this, but we need a bigger trial on children before it is integrated into practice. But this paper is a step in right direction!

Emeritus Professor of Orthodontics, University of Manchester, UK.
 Localized Piezoelectric Alveolar Decortication for Orthodontic Treatment in Adults: A Randomized Controlled Trial
Localized Piezoelectric Alveolar Decortication for Orthodontic Treatment in Adults: A Randomized Controlled Trial
so how did they measure tooth movements achieved? were measurements done during treatment or only at the end of treatment?
Corticotomy aided by piezocision or otherwise is a proven method for accelerating tooth movement
Can you explain what piezocision is, when it is done and if it is repeated please?
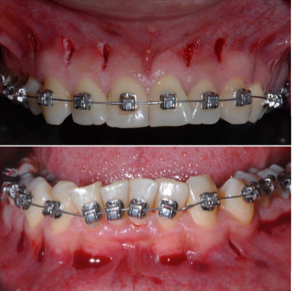
It’s sort of amazing what we are prepared to do to appease the god of straight teeth, especially in mild cases, the photo of upper teeth that you show look perfectly fine. Anyway I need a bit more convincing especially since the control group time was 1.5 yrs which seems a bit high to me for the mild maloccns described.
Would not a better way have been to have 2 matched groups (same amount of crowding at start), randomly allocated then bonded with same brace (damon by all means since no degration of elastics) by same operator and same wire size placed, then do the procedure and measure the rate of tooth movement say over 10 weeks using weekly scans. total treatment time strikes me as a risky way to measure speed of treatment since there are many variables involved which are a bit subjective
Thank you for posting this. Although the study design was reasonable, the outcomes are rather nebulous. The authors note that they used 5 criteria, but didn’t list what they were. As Dr. Kokich used to say, any claims of faster tooth movement need to be evaluated in the context of comparable outcomes. The ABO-discrepancy index, while far from perfect, provides a more quantitative means (with an established cut-off) to assess the relative outcomes of treatment between the two groups, as well as to compare how both groups would hold up against a passing ABO finish. Given the present assessment, it is quite plausible that both groups may have presented differing degrees of deviation from an optimally “finished” result. The traditionally time-consuming movements usually involve root torque, overjet reduction and occlusal fit. I’m unsure if the present study evaluated these parameters.
So, the 43% reduction needs to be evaluated in the context of these facts.
Thought readers might interested in this article in this week’s New England Journal of Medicine:
Perspective
HISTORY OF CLINICAL TRIALS
The Emergence of the Randomized, Controlled Trial
Laura E. Bothwell, Ph.D., and Scott H. Podolsky, M.D.
N Engl J Med 2016; 375:501-504August 11, 2016DOI: 10.1056/NEJMp1604635
Share:
ArticleReferencesMetrics
Audio Interview
Dr. Scott Podolsky on the evolution of the essential methods of randomized, controlled trials.
Dr. Scott Podolsky on the evolution of the essential methods of randomized, controlled trials. (08:07)
ListenDownload
The birth of the randomized, controlled trial (RCT) is typically dated to a 1948 evaluation by the British Medical Research Council (MRC) of streptomycin for the treatment of tuberculosis. But controlled clinical trials and discussions of their designs were increasingly being published in medical journals for at least half a century before the MRC’s report, which was part of a much longer history of efforts to empirically assess experimental therapies. An exploration of this deeper history offers insights into the intellectual and social forces shaping both the advent of and resistance to the controlled clinical trial as a medical research standard and mechanism for taming the therapeutic marketplace.
Trials involving experimental and control groups seem as old as the historical record itself, appearing in the Hebrew Bible and in various societies around the world, albeit sporadically, for centuries.1 As Enlightenment reasoning filtered into medicine, controlled trials emerged with growing frequency. In 1753, Scottish surgeon James Lind published a controlled trial demonstrating that a diet including citrus fruit was effective against scurvy in sailors at sea, thereby providing a touchstone for subsequent generations of researchers who gradually embraced comparative trial methods.
Loosely controlled trials increasingly appeared in the 18th and 19th centuries, often conducted by skeptics to test the utility of unorthodox remedies ranging from mesmerism to homeopathy.2 Major shifts in the social and scientific structure of medicine in the late 19th and early 20th centuries created new opportunities and demands for more rigorous clinical research methods. Hospitals expanded, new biologic and vaccine industries emerged to confront recently identified germs, chemists developed novel therapeutic compounds, and an unregulated subeconomy of fraudulent replicas of new agents flourished. All these factors motivated clinical investigators to pursue more sophisticated approaches for evaluating experimental therapies.3,4
By the late 19th century, researchers were conducting “alternate-allocation” trials, the most recent methodologic ancestor of RCTs. Conventionally dated to Johannes Fibiger’s 1898 study of diphtheria antitoxin in 484 patients in Copenhagen, alternate allocation entailed treating every other patient (or, in Fibiger’s case, patients seen every other day) with a particular experimental remedy, withholding it from the others, and then comparing outcomes. But Fibiger’s was only the most famous use of a technique that increasingly appeared in the medical literature from the 1890s onward, one that could (though only occasionally did) involve patient or researcher blinding, use of placebos for control groups, and statistical analysis of results.1
The pages of the Journal reflect this transition in research methods and the gradual but limited adoption of alternate-allocation trials to verify the purported value of new therapies. As early as 1899, a Dr. Williams described applying a glycerin–hydrogen peroxide solution “to the skin of every alternate patient” to treat desquamation owing to scarlet fever, finding shortened periods of desquamation among treated patients (1899; see box for historical Journal articles). Over the ensuing half-century, medical journals published numerous primary reports of alternate-allocation studies (most of them of infectious disease treatments), along with discussions of such studies and appeals for using this method to resolve disputes (see Selected Alternate-Allocation Studies and Discussions Published in the Journal before 1948).1
Admittedly, in 1931, James Burns Amberson and colleagues published a study in which a coin flip randomly determined which of two seemingly equally divided groups of patients would receive sanocrysin for the treatment of tuberculosis. But this study was an outlier, with alternate-allocation studies serving as the dominant model of therapeutic controlled trials in the first half of the 20th century. The number of alternate-allocation studies, however, was itself dwarfed by the number of articles promoting therapies on the basis of other forms of evidence, from laboratory and physiological justifications to case reports. Many producers of new treatments lacked economic, regulatory, or social incentives to rigorously evaluate their products in controlled trials, and many researchers simply continued relying on standard methods that were widely accepted by scientists and society.
Some researchers resisted controlled trials because they believed that participants should not be denied promising treatments by being assigned to control groups. As an editorialist lamented in 1935 regarding a trial evaluating convalescent serum for the treatment of poliomyelitis, “Parents do not have to be persuaded or urged to volunteer their children for the trial of new biologic agents — they demand them. . . . [But] means for careful appraisal were easy to devise; impossible to carry out” (1935a). That trial’s protocol called for administering the serum only in alternate cases, but researchers hesitated: “The main difficulty encountered was the inability of our special investigators to withhold this promising agent from any stricken child. . . . Our sentiment overruled our reason.”
Alternate allocation also stimulated debates about methodology. Proponents argued that alternate allocation was superior to conventional case-study methods or expert testimonials for estimating an intervention’s therapeutic value. As a 1936 editorial on the use of novel sulfa drugs cautioned, “the only way to evaluate properly a therapeutic agent of this sort is by the ‘alternate case method’ . . . even though statements of reputable physicians are impressive” (1936c). Critics, however, identified deficiencies in alternate allocation, as illustrated by a series of pneumonia trials. In 1924, Boston City Hospital’s Edwin Locke alternately assigned pneumonia patients to receive or not receive antipneumococcal antiserum and found no difference in mortality between treated and untreated patients (1924). When Maxwell Finland repeated the study a few years later, he found a benefit for the serum but admitted that “the data reveal the possibility that some choice may have been unconsciously exercised in selecting cases for treatment” (1930).
Such concerns about selection bias stemming from the ease of cheating the process of strict allocation remained the Achilles’ heel of alternate allocation and recurred in debates over a trial of diathermy for pneumonia in 1935 (1935b, 1935c, 1936b) and another trial comparing treatment with serum alone versus serum plus sulfa drugs for pneumonia in 1941. Again, Finland noted the shortcomings of the alternate-allocation schemes, pointing charitably to prevailing ethical concerns in surmising that “some unconscious selection on the part of the authors played an important role in the inclusion of the poorest subjects among the serum recipients” (1941a, 1941b).
Such methodologic concerns resonated with British epidemiologist–statistician Austin Bradford Hill, who had grown familiar with alternate allocation’s limitations while evaluating a series of MRC trials of antipneumococcal antiserum in the early 1930s. By the time he devised the MRC’s evaluation of streptomycin for tuberculosis in the 1940s, Hill was sufficiently concerned about researchers’ capacity to figure out (and hence cheat) allocation schemes that, in an attempt at frustrating such efforts, he replaced alternate allocation with strict concealed randomization of patients to treatment or control groups.5 The blinding of researchers to patients’ assignments, if at all possible, soon accompanied concealed random allocation in the emerging definition of the ideal study, in which bias was to be eliminated.2
Supported by MRC funding in the 1940s and 1950s, Hill and his colleagues impressed the research community with a series of groundbreaking RCTs. British investigators were soon followed by U.S. and other researchers who embraced RCTs as urgently needed tools for separating the wheat from the chaff emanating from an ever-diversifying pharmaceutical industry. When the U.S. Congress passed the 1962 Kefauver–Harris Amendments to the Food, Drug, and Cosmetic Act, the RCT had become an obvious methodology by which the Food and Drug Administration (FDA) could require pharmaceutical manufacturers to demonstrate therapeutic safety and efficacy before drug approval. By 1970, the FDA required that drug producers submit RCT results with new drug applications, heralding a new era with the RCT at the center of national, and expanding international, drug regulatory infrastructures.4
RCTs thus represent the most recent outgrowth of a long history of attempts to adjudicate therapeutic efficacy. Their immediate ancestor, alternate-allocation trials, emerged as part of a trend toward empiricism and systematization in medicine and in response to the need for more rigorous assessment of a rapidly expanding array of experimental treatments. Alternate allocation represented a significant advancement for addressing clinical research bias — but one that had limitations as long as it allowed foreknowledge of treatment allocation. Concealed random allocation emerged as the solution to these limitations, and RCTs were soon supported by crucial public funding and scientific regulatory infrastructures. Like alternate-allocation trials, though, RCTs expanded not only because they offered more sophisticated methods but also because they served a critical social function: screening experimental therapies before they were broadly distributed and clarifying the actual effects of medical innovations.
SELECTED ALTERNATE-ALLOCATION STUDIES AND DISCUSSIONS PUBLISHED IN THE JOURNAL BEFORE 1948
1899. Boston Society for Medical Improvement. 141:347–9.
1913. Park WH. Antitoxin administration. 168:73–7.
1924. Locke EA. The serologic treatment of lobar pneumonia. 190:196–203.
1930. Finland M. The serum treatment of lobar pneumonia. 202:1244–7.
1931a. Davis WE. The incidence of untoward symptoms following the intravenous injection of sodium tetraiodophenolphthalein in cholecystography. 205:534–6.
1931b. The clinical meeting of the Massachusetts General Hospital staff. 205:1319–20.
1935a. “Polio” vaccines. 213:687–8.
1935b. Diathermy in lobar pneumonia: preliminary report. 213:796–8.
1935c. King DS. Correspondence: diathermy in lobar pneumonia. 213:1324–5.
1936a. Curphey TJ, Solomon S. The therapeutic value of calcium salts in serum sickness. 214:150–3.
1936b. Wetherbee W. Correspondence: a discussion of Dr. Donald S. King’s criticism. 214:174–5.
1936c. Prontylin and prontosil. 215:1311.
1939. Lanman TH, Heyl HL. Empyema in children. 221:1003–9.
1940. Cutts M, Burgess AM, Chafee FH. The treatment of lobar pneumonia with sulfathiazole and sulfapyridine. 223:762–4.
1941a. Finland M. Controlling clinical therapeutic experiments with specific serums: with particular reference to antipneumococcus serums. 225:495–506.
1941b. Combined serotherapy and chemotherapy in pneumonia. 225:514–5.
1947. Artificial sunlight treatment in industry. 236:374–5.
Disclosure forms provided by the authors are available with the full text of this article at NEJM.org.
SOURCE INFORMATION
From the Program on Regulation, Therapeutics, and Law (PORTAL), Division of Pharmacoepidemiology and Pharmacoeconomics, Department of Medicine, Brigham and Women’s Hospital and Harvard Medical School (L.E.B.), and the Department of Global Health and Social Medicine, Harvard Medical School (S.H.P.) — all in Boston.
I think it’s basically creating mild inflammatory reaction which in turn will elicit osteoblasts and osteoclasts which help in faster movements, we can create inflammatory reaction by different methods, MOP,LLLT, Corticotomy, LUPUS, etc etc