Evidence based de-implementation in orthodontics. Should we stop some of what we are doing?
Evidence based de-implementation. Should we stop some of what we are doing?
Over the past few months, I have made a real effort to read the general literature on evidence based care. I came across this very interesting paper concerned with the re-evaluation of the evidence underpinning established clinical practice. It was written by Vinay Prasad and John Ioannidis, who is rapidly becoming one of my heroes with his critical viewpoints on healthcare. I found that this paper was very relevant to all health care provision and I have decided to look at this from an orthodontist’s point of view.
Evidence based de-implementation for contradicted, unproven and aspiring healthcare practices.
Vinay Prasad and John Ioannidis
Implementation Science 2014: 9:!
http://www.implementationscience.com/content/9/1/1 This is an open access paper.
In the paper they raise this very good question
“Should we continue with healthcare practices that are established that do not have an evidence base?”
They specifically base the article around three main types of healthcare intervention.
- Those that are known not to work when RCTs have been carried out
- Those for which the evidence base is uncertain
- Those that are in development
Where do we stand on these issues for orthodontic treatment?
Evidence contradicts established practice
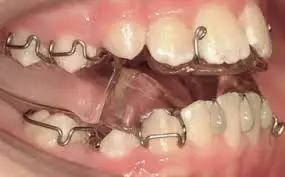 This concerns treatment where the best evidence shows no efficacy or the harms outweigh the benefits. I felt that the best orthodontic example was attempting to achieve orthopaedic or skeletal change. The evidence that we now have suggest strongly that we cannot change the young person’s skeletal pattern with functional appliances or headgear. Yet we continue to attempt this change. For example, if we consider functional appliances. We know that functional appliances tip teeth effectively and we routinely achieve good results in those patients whose skeletal discrepancy is not severe. However, in the child with a severe skeletal discrepancy should we still provide treatment with functional appliances or should we provide surgery, more effectively, when they are older? I have frequently attempted to treat severe skeletal II case in adolescence but I do also wonder if providing surgery would have been the best option. Where is the harm? Potentially this is an unnecessary course of treatment that introduces additional compensation which then needs correcting if and when orthognathic surgery is considered. As for headgear, there is no evidence to underpin that it causes skeletal change and the potential harms certainly outweighs any potential benefits.
This concerns treatment where the best evidence shows no efficacy or the harms outweigh the benefits. I felt that the best orthodontic example was attempting to achieve orthopaedic or skeletal change. The evidence that we now have suggest strongly that we cannot change the young person’s skeletal pattern with functional appliances or headgear. Yet we continue to attempt this change. For example, if we consider functional appliances. We know that functional appliances tip teeth effectively and we routinely achieve good results in those patients whose skeletal discrepancy is not severe. However, in the child with a severe skeletal discrepancy should we still provide treatment with functional appliances or should we provide surgery, more effectively, when they are older? I have frequently attempted to treat severe skeletal II case in adolescence but I do also wonder if providing surgery would have been the best option. Where is the harm? Potentially this is an unnecessary course of treatment that introduces additional compensation which then needs correcting if and when orthognathic surgery is considered. As for headgear, there is no evidence to underpin that it causes skeletal change and the potential harms certainly outweighs any potential benefits.
The evidence base is uncertain
The best example I could put forward here was the extraction of primary canines to encourage the eruption of palatally placed permanent canines. The best evidence that we have on this procedure has been developed from a systematic review on the extraction of primary canines. This concluded that there was no evidence to underpin this type of treatment. This is because previous studies were carried out with no control , for example the classic paper by Ericsson and Kurol. In other papers that they considered there were issues with steady design that the authors could not clarify. While I appreciate that this absence of of evidence does not mean lack of effect. Nevertheless our practice, in this area, is still relying on poor quality evidence. Does this do harm? Some would argue that the removal of primary canines is “no big deal”. However, this is still an unnecessary surgical procedure for a young child.
Novel medical practice
 This is when treatments are introduced with limited testing. They are then evaluated using trial methodology which then reveals that the intervention proved inefficient and possibly harmful.
This is when treatments are introduced with limited testing. They are then evaluated using trial methodology which then reveals that the intervention proved inefficient and possibly harmful.
This is a reflection of the fact that there is pressure on us to adopt new methods because we inherently feel that “new” must be “better”. In this respect, the most obvious orthodontic examples are temporary anchorage devices and self ligating brackets. For both of these treatments trials are currently underway and several of them have reported. If we consider temporary anchorage devices the reports of trials are looking interesting. It appears that temporary anchorage devices have similar effectiveness to headgear. Indeed they may be the preferred option, when you consider the potentially harmful effects of headgear. These findings are due to be reported in an updated systematic review that we are shortly to publish
But… Self legation is different. We now know that this type of bracket is no more effective than conventional brackets. But has harm being caused? The main concern is the adoption of expansion as part of the unfounded “philosophy” of treatment with sell ligating brackets. Only time will tell… Nevertheless, there is are surprisingly limited moves to “de-implement these brackets”, in spite of the evidence. Indeed the advertising is so powerful and notably non of the “advocates” have even challenged the research evidence.
What can we conclude?
In conclusion I am simply going to quote the conclusion of the paper because it is completely relevant to orthodontic care, and I cannot put it better.
“De-implementing practices reflect a recommitment to evidence-based health care. This is important for all treatments and any other intervention undertaken by people in the health professions. Strategies to eliminate a defective and harmful practice may help contain health-care spending and optimise outcomes. Ideally, the majority of medical decisions should be supported by robust data, with ambiguous decisions made only within the confines of ongoing studies. However, rational quantitative evidence may not necessarily be the only or even main factor driving health care decisions. Research to understand better the other cognitive or political factors that facilitate or hindered the implementation is thus also wanted”.
This is our challenge…
![]()
Vinay Prasad, & John Ioannidis (2014). Evidence based de-implementation for contradicted, unproven and aspiring healthcare practices. Implementation Science, 9 (1) DOI: 10.1186/1748-5908-9-1

Emeritus Professor of Orthodontics, University of Manchester, UK.
Kevin, very interesting and relevant posting.
Just some loose thoughts which come to mind.
I would like to pose the question:
Is it ethical to expose patients to interventions not supported by evidence?
I was talking with a collegue sometime ago who has a partner. He said to me:” All patients that visit my partner leave the office with something in there mouth, whereas only 50% of my patients get something!”
Are all decisions based on evidence? I wonder who rules in the land of no evidence?
You wrote:”The main concern is the adoption of expansion as part of the unfounded “philosophy” of treatment with sell ligating brackets”
Interesting typo or was it intentional?
Best wishes,
Nick
Hi Nick, thanks. You have raised a very interesting question on the ethics of exposing patients to interventions not supported by evidence. This is a difficult one as many of our orthodontic interventions are not supported by evidence! However, sensible viewpoints of the ethics of treatment could be considered on the basis of whether a body of clinical opinion would be using a certain treatment. This certainly covers a large amount of our treatment that is supported by clinical experience. It is a more difficult question when we consider new treatment. It is certainly clear to me that if a practitioner carried out treatment that caused harm to a patient and that treatment was new and not supported by evidence, then this would be unethical.
Your last comment was interesting! At the moment I have an irritating repetitive strain injury that means I have to dictate instead of type. So my typo was an intentional due to dictating. But I might leave it!
Best wishes Kevin
Hi Kevin, I’m one of those who have been using Twin Blocks for decades with great success. The design of the Twin Block and the effectiveness of the operator in getting patient compliance I feel are just two factors that studies do not account for. The image of the Twin Block included to illustrate a twin block appliance in this blog would be very difficult for a patient to wear as the vertical is jammed open way too much and the angle of the ramp is way too vertical. I can’t see how bulky the appliance is on the palatal/lingual side either. Patients have to try and eat and speak with these things in their mouth so design is everything. I also believe full lower incisor acrylic capping is essential, as is an upper labial bow for incisor control. Then I wonder how efficiently the operator trims the posterior acrylic pads during treatment to ensure the bite is opened before treatment is completed. The patient must eat with it in place and I wonder in studies how often this is accurately reported or recorded. Quite often colleagues just get to the end of their nine months quoted treatment time period and say to to patient to stop wearing the Twin Block. Retention is important in all other orthodontic treatment modalities so why do they not retain with a Twin Block? We know lack of retention leads to relapse. For 25 years I have been bonding the Twin Block together in the clinic and cutting away the cribs on the lower premolars to make it into a Bionator for the patient to wear at night for 6 months as a retainer. This to me is an essential step particularly if the Maxillary midline screw has been opened, as is usually the case.
So while evidence based studies are critically important, effectiveness or otherwise with something like a Twin Block has a huge number of variables in design, operator skill and patient compliance and patient honesty in reporting.
Regards,
Peter
Hi Peter, thanks for your comment. Your comments on the design and use of the twin block of a relevant. In our studies which we carried out some time ago we spent a large amount of time in the planning stage in coming to clear decisions on our appliance design. We did this to make the study as real-world as possible. In truth, it did not take us long to agree on our appliance designs because we were all fairly uniform anyway. I think that you have a great idea about bonding the two parts of the appliances together to use the twin block as a retainer. I will certainly do this in the future. You have highlighted an interesting issue with the interpretation of trials. When you carry out a trial to try and remove and reduce the number of variables as much as possible. However, by doing this there is a risk that you reduce the ” real-world” relevance of your findings. Again in our studies we attempted to do this and I hope that our findings were relevant, as closely as possible, to ” real-world” practice. However, it is completely up to clinicians to interpret this aspect of any study.
Again thanks for the great comments
This wishes Kevin
Thanks for a very interesting blog to read. It does make you think about Sackett’s famous pyramid of Evidence Based Medicine. Maybe this does need a revision or at least be weighted to take into account the points made by Prasad & Ioannidis.
Interesting – I always make my twin blocks without a labial bow in the upper arch. I moved to self ligating brackets by choice in 2004 and found that they did shorten my treatments by about 10%, but this was based on historic experience and audit, not randomised control and not simultaneously treated cases.
My point is this though – if there is a wide variation of success with any technique, even if the mean experience is negative, some people will find it positive. How actively would you have to assess your own experience to change your practice just because the technique isn’t successful for other people?
Stephen