Piezocision corticotomy reduces alignment time by 50%! Too good to be true?
This is a guest post by Professor Martyn Cobourne on a new trial on piezocision.
Introduction
There is currently a lot of interest in techniques that can potentially reduce orthodontic treatment time. This interest started with self-ligating brackets and superelastic wires well over a decade ago and has moved on to include vibration, light-energy and surgical assistance. Although we generally accept that neither appliance design nor vibration seems to have much effect – interest in other techniques persists. In particular, authors are publishing many studies that combine fixed-appliance treatment with different surgical procedures. These go by a variety of names but essentially involve cutting or drilling holes in the alveolus around the teeth to utilise a so-called ‘regional acceleratory phenomenon’, which is supposed to increase metabolic turnover and rate of tooth movement. My friend Greg Huang highlighted this study to me recently; a research group in Damascus did the study and looked at piezocision corticotomy. The Journal of the World Federation of Orthodontistspublished the paper.
Leveling and alignment time and the periodontal status in patients with severe upper crowding treated by corticotomy-assisted self-ligating brackets in comparison with conventional or self-ligating brackets only: a 3-arm randomized controlled clinical trial.
Al-Ibrahim HM, Hajeer MY, Alkhouri I, Zinah E (2021)
J World Fed Orthod. https://www.ncbi.nlm.nih.gov/pubmed/34688577
What did they do?
They conducted a randomised controlled trial investigating levelling, alignment and periodontal status in the maxillary arch of patients treated using fixed-appliances with or without flapless-corticotomy.
Participants: Adult patients with severe anterior crowding (Little’s index >7 mm) requiring first premolar extraction and fixed-appliance treatment.
Intervention: Empower ‘interactive’ self-ligating brackets combined with flapless-corticotomy (SLB-FC) undertaken once using a piezosurgical microsaw before initial-archwire insertion.
Controls: Conventional (CB) or Empower self-ligating brackets (SLB) only. All patients had the same archwire sequence, albeit placed at different time points.
What did they find?
They randomised 57 patients into three groups (n=19/group). Then they followed them until they could insert a 0.019×0.025-inch stainless-steel archwire.
There were significant differences in levelling and alignment time between groups with the shortest (81.89 days) associated with SLB-FC, followed by SLB (123 days) and then CB (165.25 days). This difference represents a whopping 50% reduction in duration between SLB-FC and CB groups and a 25% reduction between SLB and CB groups! In addition, the SLB-FC group had higher plaque, gingival and papillary-bleeding indices at 1-month. However, they did not find any other periodontal differences at any other stages.
What did I think?
I thought this was an ambitious and interesting study. It demonstrated the potential for corticotomy in accelerating tooth movement with fixed appliances. However, I do have some comments about the methodology and reporting.
The intervention groups
Firstly, I was not convinced of the need for two non-surgical bracket groups. This reduces sample size and provides an unnecessary additional variable. It would have been better to have two groups using the same bracket and flapless-corticotomy as the only variable.
Treatment progression
An issue with many alignment trials is optimising appointment intervals and maximising archwire progression. The principal investigator should be congratulated for trying to address this by seeing patients every 2-weeks. The main differences between groups occurred during progression from the initial 0.012-inch to the 0.016-inch NiTi archwires, a period of 124 days for the CB but only 42 days for the SLB-FC group. These are relatively light wires, and assuming equivalent irregularity, it is difficult to see how progression could have been so much faster in the SLB-FC group? The operator was also the chief investigator, and I worry that there might have been some bias concerning archwire progression. Was it really necessary to leave the 0.012-inch initial archwire in for 26 days longer in the CB group compared to SLB-FC?
Sample size
I also found myself chasing my tail when reading about the sample size calculation. This study based its estimate on Uribe et al. 2017; which, in turn, based its analysis on Pandis et al. 2008. Both of these studies investigated mandibular alignment and had relatively mild irregularity. I wonder whether the calculated sample size of n=18/group is an under-estimation based upon the fact that this study required cases with severe maxillary arch crowding?
Pre-treatment irregularity
Finally, there is one major issue. A huge omission is that the authors did not report baseline irregularity. This information is pretty fundamental for a study measuring time to achieve alignment! If we do not know whether there was equivalent irregularity between groups at baseline, the results are potentially meaningless. The more irregularity there is, the longer it will take to straighten the teeth – we all know that. So we need to know that the groups were equivalent to start with – and we don’t. In addition, despite levelling being a primary outcome, this was not measured? Given that the study ended with a 19×25-inch stainless steel archwire insertion, I am not sure the investigators can make definitive conclusions about levelling duration?
Final thoughts
My main issue with this study is that the differences seem to be just too good to be true. Thus, I think there is a high risk-of-bias, highlighted by the fact that the SLB-group aligned the teeth 25% faster than the CB. This observation contradicts quite considerably the findings of previous high-quality RCTs.
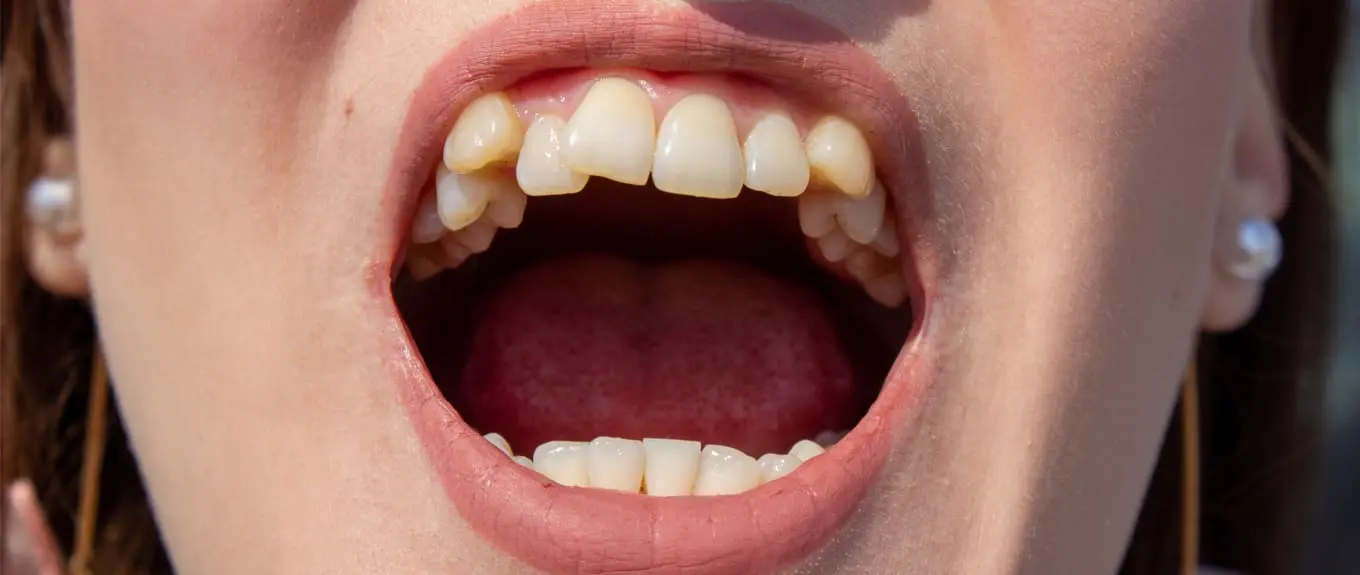
A final comment is that the observation period only represents a snapshot of overall treatment, and the investigators should follow these patients up to completion. And what did the patients think about having the fairly painful-looking flapless-corticotomy shown in Figure 1 (Ouch!)?
I have been quite critical about this study, and I feel slightly bad because I know how hard RCTs are to conduct. However, if we are going to advise patients to have surgery and orthodontic treatment – as clinicians, we need to be sure it is worth their while.
Martyn Cobourne
Professor of Orthodontics
King’s College London

Emeritus Professor of Orthodontics, University of Manchester, UK.
Why would anyone start treatment with an 012 NiTi archwire?
Why would you not progress to a larger archwire at the first possible opportunity, if the goal was to fill the slot to align the teeth?
Who, in the real world, could see patients at two week intervals?
Too much pain and no gain!
Isn’t peer-review working anymore?
I am not sure if the WFO journal is refereed?
There is NO WAY any of my patients (in my practicing days) would have consented to this type of surgical procedure as part of their orthodontic treatment, even if it “possibly” reduced treatment time! Remember “Pericision” and how many objected to that?
I think that is a fair point – and whilst times and patient attitudes change, I personally would not be keen on having that kind of intervention!