Can RME treat childhood OSA? A new systematic review!
Over the past six months, the most-discussed topic in orthodontics has been the role of orthodontic treatment in managing childhood obstructive sleep apnoea. I recognise that I have posted about this many times. In fact, regular readers will know that I have stated I will not revisit this subject unless new research emerges. This is the case with this new systematic review on RME. It was published earlier this week, and airway-focused orthodontists have enthusiastically promoted the results as high-quality evidence supporting their treatment claims. Consequently, I decided to take a closer look at it.
A team from Wuhan, China did this review. Sleep and Breathing published their paper.
Yu et al.
Sleep and Breathing, Advance access. DOI: https://doi.org/10.1007/s11325-026-03606-1
What did they ask?
“The primary object of this systematic review was to evaluate the efficacy of RME in treating pediatric OSA.”
What did they do?
They did a systematic review using standardised methodology.
The PICO was
Population.
Children with maxillary transverse deficiency who are diagnosed with OSA via overnight PSG
Intervention.
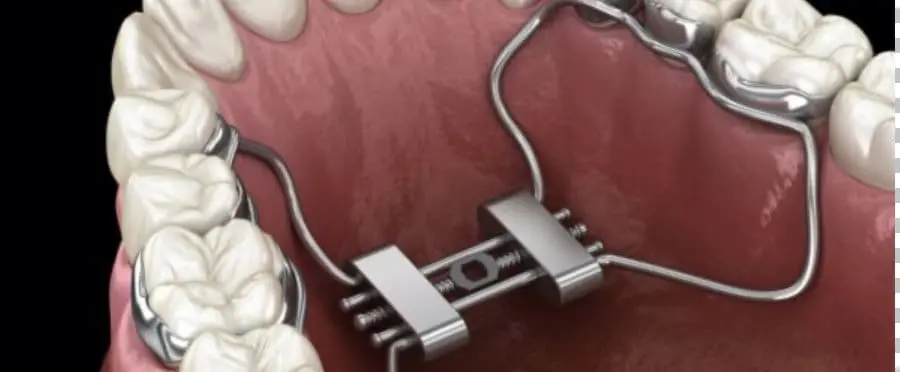
Treatment with rapid maxillary expansion appliances.
Comparison
Baseline pre-RME treatment or Watchful waiting.
Outcome.
Respiratory Outcomes and Radiological Outcomes
Study Design
They included cohort studies, cross sectional, retrospective studies, case controlled studies with a comparison or control group, and randomised controlled trials.
They carried out an electronic search, followed by identification of studies, filtering of studies, data extraction, risk of bias assessment and outcome assessment.
The primary outcome was the apnea-hypopnea index (AHI). Secondary outcomes were, sleep efficiency, peripheral capillary oxygen saturation and other patient-related outcomes
They conducted a meta-analysis using a random-effects model.
They assessed the risk of bias in all studies using the Risk of Bias in Non-Randomised Studies (ROBINS-I) tool. This was not relevant for the randomised trials they found. Finally, they appraised the quality of evidence with the GRADE tool.
What did they find?
After filtering the studies, they identified 14 suitable for data analysis. Seven of these were before-and-after studies. Five were non-randomised controlled trials, and three were randomised controlled trials.
When they performed their risk of bias analysis and found that ten studies had a serious risk of bias. They assessed four studies as having a moderate risk of bias.
Ten studies examined changes in AHI within 6 months after completing RME (mean difference: -4.04, 95% CI: -6.39 to -1.7, p = 0.0007). Heterogeneity was 93%.
Seven studies examined changes within 12 months of the intervention. These showed that the mean difference was -6.15 (95% CI, -11.66 to -0.64), p = 0.03. Heterogeneity was 97%.
They reported significant improvements in most of their other outcome measures.
The discussion was insightful because they noted a significant reduction in the apnea-hypopnea index at both 6- and 12-month follow-up. However, they highlighted that the RME did not consistently bring AHI values below 1 to normal levels.
They also highlighted that heterogeneity was very high. This diminishes confidence in their findings. Significantly, the quality of the evidence, as assessed by GRADE, was rated low or very low. They further noted that the number of high-quality RCTs was very limited, with many studies having small sample sizes and methodological flaws. Consequently, we need to be cautious when interpreting the results.
Their final conclusion was:
“These findings indicate that RME can effectively enhance the transverse width of the maxilla and improve polysomnographic parameters in pediatric patients with OSA.”
I took this from their abstract, as it is likely to be more widely read than the paper itself.
What did I think?
A relatively well-known team conducted this review. They followed standard systematic review methodology. When I read the abstract, I thought that this review could significantly contribute to our knowledge because of its very positive conclusion. However, upon reading the paper, I concluded that this was an excellent example of an abstract that does not necessarily reflect the quality of the research and content of the paper. We must remember that the overall quality of the evidence was rated low or very low.
Systematic reviews can be quite challenging to interpret due to the vast amount of information they contain. However, I have several main concerns with this review.
Firstly, they merely reported the results before and after treatment for the studies they included. They did not compare any changes to an untreated control group. As a result, it is impossible to conclude that the RME influenced AHI. This is because the results do not account for the possible effects of growth. For example, in the classic CHAT study, they found that “46% of children in a watchful wait group had some resolution of polysomnographic abnormalities.” I am not endorsing watchful waiting based on this study; I am simply highlighting that AHI can reduce spontaneously.
Secondly, they identified several included studies as being at high risk of bias. As a result, they stated that the strength of evidence was very low. Furthermore, most of these studies were cohort and retrospective studies. Again, this further diminishes the strength of evidence.
Finally, the heterogeneity in the meta-analysis was very high. They removed outlier studies to reduce heterogeneity; however, they did not publish the meta-analysis results after this removal. I have contacted the authors to clarify the situation, but I have not received a reply.
Final comments.
Over the past six months, I have been accused of being overly critical of several studies concerning orthodontics and breathing disorders. I would like to emphasise that I genuinely want to see strong evidence demonstrating that we can improve the health of this group of children with a disorder that may lead to long-term problems.
However, I have critically appraised these studies and found that many lack robust methodology and do not meaningfully address the questions we have about orthodontics and breathing disorders. I am sorry to say that this is yet another study that fails to illuminate this complex issue.

Emeritus Professor of Orthodontics, University of Manchester, UK.
My main criticism of these studies on RME is that they don’t report the average expansion achieved in millimeters. This would be a valuable clinical guideline to determine whether expansion alone is sufficient or if adenoidectomy or tonsillectomy is necessary. We lose lot of time and multiple sleep exams. What do you feel about this?
Dr Kevin O’Brien
Studies evaluating the relationship between rapid maxillary expansion (RME) and obstructive sleep apnea (OSA) have largely focused on the transverse development of the maxilla, attributing the resolution of the problem primarily to this expansion. Although the transverse development of the maxilla remains the most prominent outcome following RME, the “V”-shaped opening of the midpalatal suture also produces a butressing effect that advances the maxilla in the sagittal direction. Consequently, this increases the posterior airway volume, which is considered one of the most critical anatomical changes in the management of OSA. In the treatment of OSA, the sagittal effects of RME are therefore as important as its transverse effects.
SOS, Kevin!
You wrote, “Firstly, they merely reported the results before and after treatment for the studies they included”.
Merely? So, when T&A is done for pOSA (or other other treatment procedures in general), don’t they report results before and after treatment?
“They did not compare any changes to an untreated control group”
So, when T&A is done for pOSA, do they report changes compared to an untreated control group? BTW – residual AHI after T&A is often treated with a version of RME, which is not homogeneous, non-standardized and technique sensitive [1, 2].
“As a result, it is impossible to conclude that the RME influenced AHI. This is because the results do not account for the possible effects of growth”
A trite conclusion since you have not defined growth, on the basis of either size-change, shape-change or directionality or a combination of the same (allometry, isotropy, anisotropy). But, if kids simply grow out of pOSA then why do so many adults have the same diagnosis later in life?
“Finally, the heterogeneity in the meta-analysis was very high. They removed outlier studies to reduce heterogeneity”.
In fact, none of the studies removed intrinsic heterogeneity [3, 4] of the study samples. pOSA is not a one-size fits all diagnosis. There are known phenotypic variants, including metabolic, neurologic, myopathic and craniofacial endotypes of OSA [5]. As I wrote in a previously invited response on this blog, you are basing your conclusions on the ‘quality’ of research methodology alone, and not clinical outcomes. This is where real-world data diverges from academics. Regarding evidence-based medicine, Shackleford defined it as integrating individual clinical expertise with the best available evidence from systematic research. If you exclude clinical expertise, then it simply becomes a circular argument.
“Over the past six months, I have been accused of being overly critical of several studies concerning orthodontics and breathing disorders. …….. However, I have critically appraised these studies and found that many lack robust methodology …. I am sorry to say that this is yet another study that fails to illuminate this complex issue”
And you vent this on a blog? A blogger carries the same weight as the much-maligned YouTube video influencer. If you have genuine concerns, then the academic instrument is to write the Editor of the peer-reviewed journal that published the study outlining your concerns. Otherwise, if orthodontics is a football game, then a blogger is a cheerleader not a referee.
1. Singh GD. Maxillary appliances for the treatment of moderate obstructive sleep apnea: adjustability and mechanisms. Trials 2026; 27:68.
2. Singh GD. Craniofacial growth and development: Does epigenetic deformity follow dysfunction? Amer J Orthod Dentofac Orthop 2026 (in press).
3. Singh GD, McNamara JA, Lozanoff S. Craniofacial Heterogeneity of prepubertal Korean and European-American subjects with Class III malocclusions: Procrustes, EDMA and Cephalometric Analyses. Int. J. Adult Orthod. Orthog. Surg. 13(3): 227-240, 1998.
4. Singh GD. Craniofacial endotype of obstructive sleep apnea: Spatial matrix hypothesis. Sleep Breath. 2026;30(2):106.
5. Singh GD, Battle J. Integrative treatment of obstructive sleep apnea: principles and practice. J Clin Sleep Med. 2025;21(9):1591-1596.
Thanks for your comments and I have noted them.
Dear Professor O’Brien,
I agree with your excellent analysis on the OSA/RME study.
OSA is a very serious condition in children and coordination of care with ENT/Sleep Studies/ pediatrics with the treating dentist is essential for optimal results.
If the child has a space deficiency, it makes sense that RME could help in coordination with
The above medial specialities. Maybe these kids with OSA could be placed as add on patients to the monthly cleft palate clinic “team” to coordinate care?
Dear Professor,
This in my very humble opinion is exactly the level of critique that is needed in addressing such critical questions. Especially when we are looking at treating young children and the weight of the consequences of our treatment(s)/ lack there of.
Thank you for always being the voice of reason and critical thinking in this age of trends and fads.