To extract or not; the constant orthodontic dilemma?
To extract teeth or not; the constant orthodontic dilemma?
One of the most important decisions that we take in orthodontic treatment planning is whether we need to extract teeth or not. This post is about a recent study that evaluated aspects of this decision.
I find it surprising that after many years of research, and practice, that I have limited evidence to use in the decision to extract teeth as part of my treatment. As a result, the decision that I may take about extractions is mostly based upon clinical experience. At this point, I would also like to point out that there is no evidence that extractions cause harm. I have discussed this before.
The Angle Orthodontist published this paper. This is an open access journal and you can download the whole paper.
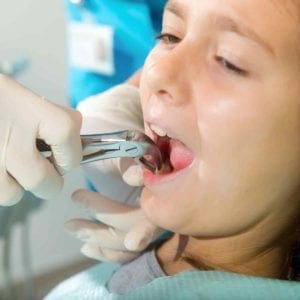 Influence of clinicians’ experience and gender on extraction decision in orthodontics
Influence of clinicians’ experience and gender on extraction decision in orthodontics
Niousha Saghafi et al.
Angle Orthodontist: Advanced access.
In their introduction, they pointed out that most of the controversy about the extraction decision was concerned with borderline cases. Previous studies studies have showed marked inconsistencies for this type of case.
They did this study to find out if the experience of the operator had an effect on the extraction decision for borderline cases. They also wanted to find out if gender and place of education had an effect.
What did they do?
They carried out a study in several “steps”.
Step 1
They took a sample of treated cases from the graduate clinic records. They used the following inclusion criteria
- Complete records
- Orthognathic profile
- Class I molars and canines
- Crowding of between 4-8mm
They initially identified 8 cases and used them in a pilot study. The investigators put these into a computer survey and showed these cases to 16 Faculty members and 15 residents and asked them to state whether they would extract or not? They then used this data to identify a final sample of three cases in which the examiners could not agree on the extraction decision. These were defined as borderline cases.
Step 2
This was an ambitious data collection exercise. They sent a survey to a large sample of 2005 orthodontists who were active members of the AAO. The first part of the survey gathered demographic information on the orthodontists. In the second part, they sent the case records to the orthodontists and asked them to record their treatment decisions. Finally, they asked them whether their decisions to extract had reduced over time.
What did they find?
They got a response rate of 253/2005 (13%). Of the respondents 28% had less than 5 years experience, 32% were in the 5-15 years experience group and 40% had greater than 15 years experience.
When they looked at the non responders they found that more clinicians in the least experienced groups responded. Importantly, clinicians with more than 15 years experience were less likely to respond.
Finally, there was a different response rate for each case.
They presented a large amount of relevant data. So that I can be brief I have extracted the relevant data into this table.
| Before Treatment | I month pre-op | 1 month post-op | |
|---|---|---|---|
| OOQL | |||
| Surgery 1st | 57 (51-62) | 22 (20-23) | |
| Control | 52 (46-57) | 60 (14-21) | 29 (24-33) |
| OHIP | |||
| Surgery 1st | 16 (12-19) | 2 (1-3) | |
| Control | 13 (10-15) | 18 (14-21) | 3 (1-4) |
This showed that most clinicians preferred a non extraction approach.
Their overall conclusion was
“More clinicians with greater than 15 years experience preferred extractions than clinicians with less experience”.
Finally, 24% of the respondents believed that extraction rates had decreased. This was due to change in treatment philosophy (48%), aesthetic beliefs (31%) and patient choice (21%).
What did I think?
I thought that this was a simple study that attempted to answer a difficult question. However, we need to consider whether the investigators achieved their aims. I think that they did, to a degree. As with all studies, there are some shortcomings. We need to evaluate whether these are so great that the findings do not add to our knowledge. This is my interpretation of these issues.
Firstly, they used case vignettes. Some would suggest that this is not a “real world” situation as it does not reflect the clinical assessment. Nevertheless, orthodontists are perfectly capable of coming to decisions based on full records. As a result, I feel that the use of cases was both satisfactory and practical.
My major concern is with the low response rate (13%). I think that we have to consider whether the sample of respondents may not be representative of a population of “typical” orthodontists. This is a considerable limitation and I wonder if we can conclude that the findings are only relevant to the respondents.
Finally, the authors pointed out there was not an equal number of extraction/non-extraction decisions made by the orthodontists. This may mean that outside of Seattle, the cases were not really borderline! But I am not familiar with USA orthodontic demographics and perhaps I am being a little mischievous?
Overall summary
If I consider these issues, I still feel that it was interesting that the older practitioners were more willing to extract. This may be due to their clinical experience in treating more extraction cases than the younger practitioners. As a result, they were not concerned about taking a this decision because they could manage space closure. Alternatively, younger practitioners may be more influenced by their recent training. This may be based on the current trend to treat more cases on a non-extraction basis.
I also think that it is important to remember that there is limited research on the need for extractions in borderline cases. We know that no harm is done by extractions, if the mechanics are correct. We also know that non-extraction Class I treatment is easy. Perhaps the younger orthodontists are taking the easy option for them and their patients. There is, of course, nothing wrong with this approach.
In order to finish, I need to put forward a word of caution. This is needed before all the non-extraction at all costs, breathing consultants, jaw expanders and orthodontic oral physicians get excited. This paper was based on borderline cases. There is no doubt that some cases are clearly non-extraction and others are extraction. The orthodontist who never extracts may be causing the same amount of harm that they accuse those who routinely extracting.
And so the wheel keeps turning….

Emeritus Professor of Orthodontics, University of Manchester, UK.
Kevin,
How patronizing can you get?
“In order to finish, I need to put forward a word of caution. This is needed before all the non-extraction at all costs, breathing consultants, jaw expanders and orthodontic oral physicians get excited. ”
Even though it was a small, possibly skewed study, is it not possible that the more recently qualified orthodontists have read, and become exposed to information which makes them reluctant to extract?
Apart from supernumerary teeth and extreme anatomical conditions, the human body doesn’t have any ‘spare parts’ that can be removed at will, by a ‘specialist’ who believes what he/she was taught many years ago and steadfastly refuses to look at other options. Optimal Patient Care is not Optional Patient Care. There is an increasing number of orthodontists here in the US who are starting to see ‘the writing on the wall’ and making a point of expanding their knowledge base. One of America’s best loved philosophers, Wayne Dyer, made this statement.
“The highest form of ignorance is when you reject something you don’t know anything about.”
Hi Roger, I am afraid that British sense of humour was lost on you…
Hello, Kevin. From this side of the Atlantic, as I see it Roger Price’s use of Wayne Dyer’s quote is misplaced and inappropriate. Minimally, Roger sees fit to read your reviews.
I am agree with your word caution should be taken to decide for extraction or not ,if other parameter like over jet ,soft tissues profile and inclination is Normal.
Agree with your final comment Kevin that a total non extraction philosophy is not feasible or correct .
However , I have a fair amount of migraine , neck and back ache cases I see and treat successfully by disoccluding and advancing the mandible forward a tiny amount and it relieves symptoms . (As it did with myself, as a postextracton case.)
These patients are often inappropriate upper premolar extraction cases, with slightly distalised mandibles.
So have to disagree it does no harm , despite you saying no evidence.
Retracting canines causes loss of facial canine eminence . We all see this happen and it nearly always worsens facial appearance.
Again I realise you have papers that say this is insignificant I beg to differ.
A good top lip is the foundation of a beautifull face and to extract to reduce overjet is a clinical mistake frequently made in my humble opinion.
The upper anteriors should not be retracted to a pathologically placed mandible , even if the mandible will not fully function forward.
The place it is ok to extract upper premolars is NOT to relieve crowding, but when the patients top lip is already to full and they have a prognathic profile.
This is Very Very rare / unusual in caucasions.
Glad to see extraction rates falling again , back to Edward angles original philosophy of do no harm .
Great post . Hope you don’t mind me disagreeing with a few points.
Regards Peter
Would it be worth trying to publish a series of these cases where the neck/back ache etc has been resolved following orthodontic treatment…?
Sounds interesting.
It’s amazing to believe that we are still discussing this basic issue. I’m not sure that patients only fall into 2 categories either since there is a third one of “try non extn and then extract if necessary” or therapeutic diagnosis. The extraction decision a few months into treatment being based on appearance (ie a bit horsey) or ceph appearance (a bit proclined) or inability to align the teeth. I find myself doing this more frequently since you can really justify the extraction decision if you have already tried the alternative.
Completely Agree . I used to have this at the back of of my mind as an option when starting a very crowded upper arch , And I have NEVER have had to retrospectively extract . The case always sorts itself out to the parents complete amazement. having been told their child is a definite extraction case elsewhere.
Hugely crowded arches are absolutely routine non extraction cases for me now. Only true prognathism warrants extraction and these cases paradoxically are not crowded at all . They usually have well aligned straight arches but need retraction to ease a prognathic profile . (more commonly Asian or African genetically, rarely Caucasian). Extracting to relieve crowding is usually in correct diagnosis, as the facial profile has not been considered.
Sassonis facial arc predicts where anteriors should go and Caucasians are nearly always retro gnathic of this, especially in crowded cases.
Expand Expand Expand !!! ( Sorry KEV !)
As long as treatment goals include facial balance, optimal incisor position, periodontal and TMJ health, extractions will always be a significant part of orthodontic treatment. As you noted, untrained and inexperienced practitioners are often unable to manage space closure. In addition, they are also likely to succumb to pressure from all the pseudo-science and specious reasoning that seems to be endemic nowadays. If anything, new information should make one more willing to extract in borderline cases!
Why is that we have to discuss hypothetical scenarios as if patients do fit into either black or white? At the end of the day decision to go either way is a combination of what we know and its published (goor or bad), what the patient’s desires/beliefs and needs are, and our our clinical experience/expertise. These three pillars are never equal for any given patient. We have such scarcity of long-term data that every opinion is respectable until proven wrong. I am certainly doing more “therapeutic diagnosis”. Not efficient but clearly fair for all the involved parties. For any given patient it goes from “i have no idea why this doctor is taking about” to ” now I can see what he/she referred to”. Proper, underline proper, informed consent is a cornerstone concept that we seldom discuss about.
You’ve done a great job of summarizing this clinical study as submitted by one of my residents, Niousha Saghafi. (Of course, as a co-author I am biased)
I was pleased to see it has been published in spite of the difficulty we had in obtaining the cooperation of a very large sample of more than 2,000 AAO members. Only 13% fully complied with our request to plan treatment for 3 patients selected with 4-8 mm of crowding. I believe this was primarily due to the fact that it required about 30 minutes to analyze the complete records of these patients. As stated, these cases were selected because they were slightly “orthognathic” in facial appearance. All patients had a full dentition and one could expect to see overall expansion of the arch if treated non-extraction. Current studies show that when clinicians decide to extract premolars (either 1st of 2nd) with this much crowding, they do so to improve the face. See the reference: Janson, et.al. “Influence of premolar extractions on long-term adult facial aesthetics and apparent age.” European J. of Orthodontics – 2016. The authors of this study concluded that “Premolar extractions, when correctly indicated, usually improve facial attractiveness.” I have attached an Invisalign prediction of how teeth move when aligned non-extraction with 4-8 mm of crowding. Do you routinely want this much facial change not to mention the potential problems with mandibular arch stability? In our study I was pleased to see that the more mature orthodontists were somewhat more willing to extract.
I was surprised at the low rate of response. I was also surprised at the analysis of the non-responders compared to did-responders. Can you give me an idea of the number of AAO members that support research via donations, as I am surprised so few would support a credible project with spare time?
And did you get a better response from your own graduates and post-graduates?
Stephen Murray
swordsortho.com
One more reason for seasoned orthodontists willing to extract more might be that they have seen futility of previous non-extraction treatments(done by self and others). Re-treatment with extraction is answer, many a times in such cases. Ageing and third molars possibly lead to protruded anteriors, calling for a re-treatment.
Kevin,
Thanks for taking the time to digest and discuss this article. It is a good vehicle to allow some thoughtful discussion on the 120 year old extraction-non-extraction debate. We have talked so much about this subject that we fail to see how the language and the word choices we use actually are part of what keeps us from coming to a consensus on the issue. It also allows naysayers to heap everything from migraines, loss of canine eminence to sleep apnea at its door step. I think it is only a matter of time before climate change will some how be connected to extractions for orthodontic reasons. (Fake or not….)
We need to stop talking about extractions as a “cause” of anything. The only thing extractions “cause” is space in the dental arch. Everything good and bad that happens after the extractions is “caused” by the orthodontist moving the teeth. In the case of facial change, if you do not want facial change yet there is crowding, remove teeth and use mechanics that allow you to treat the crowding without changing the position of the anterior teeth. Presto, no facial change.
What I am saying is we have gotten used to using sloppy language and imprecise terms to describe our very precision driven profession.
When someone says “extractions ruin faces” then every child in the world is running around “ruining their faces” by “extracting” their (deciduous) teeth! Of course that is not what we mean…….well then, we actually need to start being very specific about what we mean when we talk about this stuff.
Orthodontics is about placing teeth in very specific places to achieve desired results. We need to start talking in very specific language rather than the vague generalities we use so often that we are deaf to how silly the debate in those terms really is.
The response rate is pathetic! What is wrong with orthodontists not wanting to help out colleagues to do their research. All who read this, the next time a colleague asks you to answer a questionnaire for research purposes, please take the time to answer!
The real question that should have been asked was which teeth to extract, realising that third molars are teeth, not whether as most patients lose at least 4 teeth.I treat most borderline cases with second molar extractions to produce stability with no loss of lip support. This means managing the third molars eventually but after 35 years experience that is not a problem. Of course one must follow patients through but that is a pleasant experience as the results are esthetic and stable.
Hi Kevin, it’s a shame about the low numbers response but I’m glad you still took the time to present this.
I’m also pleased to see ‘Specialist’ Orthodontic trends are getting closer & catching up those set by General Dental Practitioners doing Ortho. with almost no extractions for decades now.
What has been the general trend over the last 3 decades for Orthodontists extracting teeth? I’d estimate 45-35% range 20 years ago, 35-25% 10 years ago and around 25-20% of Orthodontist’s cases now.
Thus I think we can all agree this effect is trending in the right direction.
Whilst this study may be too small to be conclusive, it nevertheless throws up some interesting questions, especially the significant difference between prescribing between the younger Specialists and the Older ones.
I wonder if the stats will be Orthodontists only extract in 10-5% of cases in another 20 years……?
I also wonder if Lateral Cephs will no longer be taken by Orthodontists or only very minimally at 1% level then too, given today’s trending evidence is also Lat.Cephs make little/no difference to clinical prescribing or outcomes and are more administrative, defensive or research purposed, but that’s another ‘modernising’ issue waiting for catch-up, some might say 😉
Anyway the above trend is progress and whatever one’s own preferences, it is to be welcomed.
Best wishes,
Tony.
90% of my patients are Chinese and the extraction rate is 90%. The other 10% are Causasians( expat community) and the extraction rate is only 10%. Clearly based on my practice profile, you do non extraction on Causasoid based cases.
Good point. About a fifth of my cases are for aligning (mainly) impacted canines, usually non extn, this doesnt mean that everyones should be. Could it be that all this differing opinion is because of the different population groups that we see? At leadt partially. Maybe those of us who treat everything non extn are extrapolating from their experience with their patients in their neck of the woods, to everyone else.
In our demographic, extraction rates are almost 70%. So definitely not going down by any means. Comments by non-orthodontists are likely biased and conflated due to a lack of knowledge/training on Tx goals, mechanics, outcomes etc. Based on all the re-treats of non-extraction cases that have relapsed severely and now need extractions, one can safely say that the trend is definitely in the wrong direction.
Hi Kevin Thanks for the article. I was a little confused by this statement: “The orthodontist who never extracts may be causing the same amount of harm that they accuse those who routinely extracting,” and wondered if you could provide some clarity for me? Specifically could you comment on how not extracting or indeed not treating malocclusion causes harm? And how does orthodontic treatment without extraction (in certain cases) cause harm? Could you provide me with some particular cases studies to indicate this? Thanks greatly F
Hi Kevin thanks for the article. I wondered if you could provide comment on the following statement as it intrigued an confused me some: “The orthodontist who never extracts may be causing the same amount of harm that they accuse those who routinely extracting.” more specifically, i’m aware you’ve mentioned a piece of research suggesting extraction doesn’t damage facial profiles, but could you comment on how not extracting and indeed not treating a patient causes harm.In what way does it cause harm? And how (in certain cases) the decision to provide treatment not inclusive of extraction causes harm where extraction otherwise wouldn’t. Do you have some case studies to indicate this. Alternatively are you simply suggesting that both non extraction and extraction cause no amount of harm if done correctly? If so, why extract? Regards F
Thanks for the question. You have asked several complex questions and I think that it is best to consider your last one. It is clear from the literature that I have reviewed in other posts that it is not the extraction that causes the problems, it is the mechanics that are used. That is poor mechanics are more likely to cause harm than the extraction decision. As a result, the extraction decision argument is somewhat redundant.
Kevin thanks for the response. If i a may just to clarify my confusion.: How does not extracting cause harm? Are you suggesting therefore if orthodontics is performed correctly there should be no need to extract?
thanks F
You can theoretically cause harm by overextending the dental arches leading to a potential loss in the bony support of the teeth. No I am not suggesting that there is no need to extract teeth. Extractions are necessary when there is a severe amount of crowding so that we do not move teeth off the bone or make our patients look as though their teeth are too far forwards.
Hi Kevin thanks very interesting and so if I may, what is the underlying cause of needing to extract, too big teeth or too little bone? And what causes that to happen? F
Essentially there is not enough space for the teeth so it is likely to be combination of genetic and environmental factors. But the exact cause is not known
Could you point me to some research that has been conducted into this matter. Thanks F
This is a summary that I came across by a simple search
http://cdn.intechopen.com/pdfs/31376/InTech-Genetic_factors_affecting_facial_growth.pdf
Thanks very interesting. I’m in agreement i do not think that this pathology is solely the cause of a genetic trend towards ‘not enough space’. Certainly I can understand how environmental factors may precipitate certain growth changes and a patients genetic traits may elucidate particular patterns of malocclusion. What environmental factors have you established as being relevant to this pathology? F
Thanks very interesting although I’m concerned that I made a simple google search and this was the first article that came up, I was hoping to be directed to some more concise research, perhaps something I could not have found on the first page of google? Do you have any other recommendations for me in that sense?
I’m in agreement I do not think that this pathology is solely the cause of a genetic trend towards ‘not enough space’. Certainly I can understand how environmental factors may precipitate certain growth changes and a patients genetic traits may elucidate particular patterns of malocclusion. Given that every pathology is a combination of genetics and environment, what environmental causes have you established as being relevant to this pathology? F
Thanks for the comment. One concept that we all need to accept is that malocclusion is not a disease, it is a variation from normal. As a result, it is not correct to call it a pathology. The research in the aetiology of malocclusion is not strong and much is based personal opinion and theory. Along with some interesting but now old experiments. I choose this paper because it was recent and fairly well written. The most obvious enironmental causes are the tongue and soft tissues. However, these are very difficult if not impossible to modify. As far as I know there have been no trials that have evaluated this question.
Do you inform your patients of the likely environmental causes and recommend that they investigate how best to address factors relating to the tongue and soft tissues?
Another variation from normal therefore would be the growth of the whole jaw downward, inward or backward, and we know that sleep apnoea is treated most successfully by advancing the maxilla, (I make note: advancing the maxilla into a more ‘normal’ skeletal variation) and always requires orthodontics.
I’m sure you’ll agree that one can have multiple ‘variations’ from normal and they do not act elusively of one another. How do you factor in this during pre-treatment assessment?
I do all this as part of my diagnosis, treatment planning and consent. I am not sure where these questions are going?
Its a relief to know that you only treat people who have mild malocclusion and no other possibly associated problems such as sleep disordered breathing et al. And that you appropriately look for identify and direct those with possible/probable sleep disorder breathing or the identifiable factors present on examination of the growth of the jaws to the necessary specialists rather than treat wonky teeth solely as one symptom and ignore what else may be going on with the patient. Your patient range must be very small and generally of the same type of mild class I malocclusion with good skeletal relationship that wouldn’t need extraction. F
I really do not know what point that you are trying to make here. For the last 30 years I have only treated complex problems requiring combinations of surgery/orthodontics, complex treatment mechanics and children with complex medical disorders. I think that I know what I am doing. I have a question “are you a dentist”?
No Im not and i’m more than entitled to share and express my concerns as a patient and member of the public. If discussions were confined solely to those apart of the same vanguard of opinions, nothing constructive will be discussed.
I apologise for my resolve, I do not want to discredit your career or work with children but my interpretation of your many comments regarding no link between breathing and malocclusion, the continuous deridement at every possible opportunity of those specialists who disagree with that opinion suggested to me that you focus solely on malocclusion exclusive of associated factors like many, as is my experience and the experience of many of my colleagues, practising orthodontics. Do you disagree? As such, any statements that you make that may need clarification for the interests of the public, I will continue to as such.
Thanks and I was only asking. There is no need to be so aggressive.
Thanks for your other comments. I am not being disparaging about other views in my posts. I simply highlight issues of lack of evidence in the treatments that are promoted by the specialists that you admire. I suppose that I am doing this to protect the public (i.e.you) from treatments that may not work. Who should you believe? I am an independent scientist with no monetary interest in promoting and selling treatments…
At some point of time, we as orthodontists, have to get down to correcting the malocclusion. As part of that correction, extractions might be indicated. No amount of instead of waxing eloquent about genetics, the environment, multiple variations from normal etc. is likely to provide a viable solution to an existing condition. While it is interesting in theory, these are very abstruse concepts with no clear linkage to the existing malocclusion. These type of changes occur very slowly and over time.
So, where is the evidence supporting a link between breathing and orthodontic extractions? There is certainly data to the contrary. Perhaps we should all decide to concoct fantastical theories far divorced from reality? Who is the arbiter of fact, and more credible? Gurus espousing financially conflicted opinions, or independent research from scientists? The fact that this is still being discussed in this day and age is troubling….