Back to Basics: MiniScrew-Assisted Maxillary Expansion (MARPE)
This is the second of three posts by Martyn Cobourne on the current state of evidence on expansion. In the first of these posts, he discussed the basic principles of maxillary expansion and assessed the evidence base of conventional RME. In this post, he looks at the use of MiniScrew-assisted expansion devices.
Background
In recent years, the use of fixed anchorage has become widespread in orthodontics, which, combined with the relative ease of placement and high rates of success for MiniScrew anchorage in the anterior maxilla, has led to the development of tooth and bone-borne; and, more latterly, exclusively bone-borne expanders, such as the MiniScrew-assisted Expander (MSE) and MiniScrew-Assisted Rapid Palatal Expander (MARPE).
Compared to some parts of Europe and the rest of the world, orthodontists in the UK have yet to adopt these types of expanders to quite the same extent in their routine clinical practice. However, we believe these appliance systems represent the future – so this week, we will discuss the evidence base.
MARPE also appears to have a high success rate and can produce significant differences in post-expansion skeletal and dental dimensions over the short-term (+3.34 mm and +4.56 mm along the intermaxillary suture at PNS and ANS, respectively; +3.96 mm inter-canine width; +4.99 mm inter-premolar width and +5.99 mm inter-molar width); these essentially follow opposing pyramidal patterns with anterior skeletal expansion > posterior but molar dental expansion > canine; MARPE seems to produce twice the amount of skeletal expansion compared to dental.
MARPE can also produce significant differences in post-expansion skeletal and dental dimensions when carried out in post-adolescents and adults (+1.11-4.50 mm skeletal expansion; +2.86-5.83 mm inter-canine width; +5.33-6.09 mm inter-premolar width and +5.40-8.32 mm inter-molar width). This makes MARPE a viable alternative to surgical-assisted RME (which we will discuss in a further blog).
Which is better? Conventional RME or MARPE?
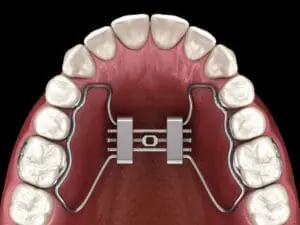
Tooth-borne or conventional RME has been used successfully for many years, but some apparent disadvantages are associated with applying an orthopaedic force to the maxilla via the dentition. Inevitably, it produces some tipping and buccal expansion of the supporting teeth, potentially reducing the overall skeletal expansion achieved.
In addition, these tooth movements are susceptible to relapse and can be associated with some detrimental effects, such as loss of attachment and root resorption. Applying the orthopaedic force directly to the maxilla with a bone-borne appliance circumvents the need to use direct pressure to the dentition, which should maximise the skeletal expansion and minimise any detrimental effects associated with the teeth. What does the evidence comparing these different approaches say?
What is the evidence?
- MARPE has been associated with more significant skeletal expansion along the intermaxillary suture at the anterior nasal spine (+1.21 mm); first premolars (+ 1.13 mm); first molars (up to +2 mm), and PNS (+1.14 mm); and increased dental expansion at the first molars (+ 0.75 mm) with reduced buccal inclination of first premolars and first molars (-6.06 and -3.17 degrees, respectively) when compared to conventional RME).
- MARPE seems to have other advantages over conventional RME, including the increased opening of the intermaxillary suture, increased palatal width, reduced buccal tooth inclination and adverse periodontal effects (although it does not eliminate them).
- MARPE is more invasive and involves a surgical procedure under local anaesthetic. It is undoubtedly more expensive than conventional RME, and the latest protocols also advocate CBCT scanning to improve the accuracy of implant placement (let’s not continually dismiss the potential dangers of routine CBCT usage). https://kevinobrienorthoblog.com/brain-cancer-after-ct-examinations-of-children-and-young-adults/). Data on patient-reported outcomes for all types of maxillary expansion are generally lacking; however, whilst these procedures are all associated with some discomfort and minor inconvenience for the patient, they all seem to be generally well tolerated.
Conclusions
Overall, the evidence base for RME is low-level, and this is particularly so for MARPE. Despite many systematic reviews, there are few good-quality RCTs, much heterogeneity between studies, and little long-term follow-up. Maxillary skeletal expansion is readily achievable using a variety of appliance designs and protocols, but MARPE seems to be the future. First, however, there is a need for some high-quality clinical trials to investigate further and refine these appliances.
A version of this post appeared first on Martyn Cobourne’s and Andrew DiBiase’s Evidence-Based Orthodontic Facebook Group.

It would be nice to know the results distributed by age (adults vs young teens). Additionally, what are some of the side effects seen (especially in adults) when things go wrong with MARPE.
are the results of this study immediately after the removal of expanders? Were the amounts of expansion using both styles the same?