Back to basics. Ten top tips on alignment.
This week, we return to the Back-to-Basics series. In this new post, Padhraig Fleming gives us his top ten tips on orthodontic alignment. It is good to get a reminder of some basic clinical aspects of our care.
Introduction
I posted some disparate thoughts concerning space closure in January. We have decided to do something similar regarding initial alignment. I appreciate that I am doing this in the wrong order, but hopefully, this is of interest and use.
As is the case with space closure, there have been many excellent studies addressing the effect of appliance variations and adjuncts on the efficiency of initial alignment. A number of these were, for example, undertaken to assess the effectiveness of putative approaches to hastening treatment (e.g., non-surgical adjuncts, surgical adjuncts and self-ligation) using the efficiency of alignment as a surrogate measure of overall treatment efficiency. By and large, these have not shown particular advantages associated with a range of adjuncts. Bracket type and NiTi wire generation or make-up also appear to be secondary. Yet, we do know that the ‘time to align’ is variable.
What governs this? The major contributors are the operator and the patient. Clearly, the patient is the patient. I firmly believe that the decisions that we make as the operators are, therefore, pivotal in the efficiency and outcomes of treatment (from planning through to finishing and detailing). Often, these fundamental decisions and technical details get lost in the magnetic maelstrom of gadgets and their marketing. It is also important, I think, to highlight that ‘efficiency’ is probably a better term than simple ‘speed’. The former implies getting to the same end-point (an optimal treatment outcome), while ‘speed’ does not, and the latter may come at the (not insignificant) cost of an inferior outcome.
As with space closure, there is evidence to support some but not all of what follows (and I will highlight these where they come to mind); however, I have to highlight that much of the following has no evidence base, and some is relatively intangible.
So here are 10 top tips:
1. Bracket Position
Think about what we are aiming to do. We are aiming to align the bracket slots. Clearly, if we position the brackets correctly, the teeth will align with the slots. However, alignment of the slots is fundamental if we are to progress through our archwires and, therefore, address further treatment objectives efficiently.
2. What are your objectives?
Think about the objectives and the following appointment: This seems like a truism but it is important. We have lots of options when we place brackets and engage wires, particularly in the presence of crowding. Should we engage fully or partially? Should we place the bracket on the LA point (or as close to it as possible)?
Typically, I would say fully wherever possible and I try to place the brackets on the LA point. However, in the presence of crowding (e.g., in the lower anterior region with reduced inter-bracket span), it may be sensible to accept slightly off-centre positioning to allow for full wire engagement (with planned repositioning at a subsequent visit). This approach will at least lead to wire deflection and, ultimately, therefore, tooth movement. Overly ambitious ‘optimal positioning’ might, however, render us unable to engage/deflect the wire sufficiently, causing relative stagnation.
3. Engage fully where possible:
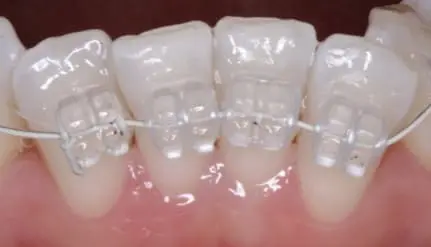
As a rule, fully engaging the wire is essential if we are aiming to progress (increase wire dimensions) at the following visit (although there are exceptions to every rule).
4. Conventional or self-ligating brackets?
I think we are well aware of the evidence on this, and I won’t revisit it. There is no evidence that blanket use leads to more efficient tooth movement. Prospective studies have almost uniformly failed to show a difference between conventional and self-ligating brackets, although practitioners do cite initial alignment as a time when SLB use may be of some benefit (Prettyman et al., 2012). Nevertheless, I have advocated for the local use of self-ligation for many years on particularly rotated or displaced teeth, as the benefit of secure, robust ligation can be very useful. Specifically, I gravitate towards self-ligation on rotated premolars, displaced lateral incisors and rotated canines (on these teeth, in isolation). The message here is to keep an open mind and to be responsive to the dictates of the malocclusion.
5. Active mechanics or not?
I have a tension on this one. I teach to use these sparingly. In practice, I use them more than I teach (And one of my mantras is to teach what we do wherever possible). This rather contradictory and conservative approach is based on the risks of getting active mechanics wrong on early wires. However, if I see reciprocal rotations (perhaps central incisors both rotated mesially), I may add a light coil spring. Equally, in the presence of rotated teeth, I may add a chain. I will terminate the chain on teeth needing rotation towards each other. If this set of circumstances does not exist, I will pit a tooth with larger anchorage value (e.g., a canine) against the incisor that I wish to derotate in the expectation that we will get preferential derotation of the tooth with lower anchorage value.
6. Consider wire dimensions.
When I trained, one of my supervisors advocated starting with 0.016-inch NiTi (in a 0.022-inch slot) unless otherwise stated. Given the flexibility of newer-generation NiTi wires, I would not recommend this. I try to start with a lower-dimension wire but fully engage it to align the slots. Given sufficient time (and careful engagement), there is often no reason why progression into 0.018-inch SS, large dimension round NiTi or even rectangular NiTi may be possible at the subsequent visit (pending on the extent of the malalignment and dictates of the residual issues).
7. IPR or not?
This question speaks to a more fundamental issue—space requirement. However, if we have determined from our space plan that IPR is required, some sparing IPR can be very helpful at the outset. Clearly, this may minimise the risk of round-tripping in crowded cases. I also like to undertake IPR incrementally in adults with thinner periodontal phenotypes.
8. If in doubt, reposition.
I am a huge advocate of doing what we can to progress treatment at every visit. We should be vigilant of the need for repositioning. I have seen lengthy threads on this previously on Facebook, and I can’t help but think that the timing of repositioning can be a ‘practice management’ decision. It should not be. It should be a patient management decision, and we should, I think, try to address these issues early. I like getting brackets right early as it is much neater. Moreover, we know that repeated wire bending isn’t always consistent or perfect (and limits our flexibility during finishing). Equally, certain wire bends are a little less predictable. Specifically, rotational correction necessitates wire bending that tests the ligation (the weak link of the bracket-wire interface). Therefore, rotational issues related to positioning errors are best dealt with early.
9. Record your repositions.
Regular review and audit of our work is clearly good practice. I reposition many attachments, and it is important to appreciate which ones I get wrong most often. Recording and regular audits of these are really useful. Simply record the tooth involved and the type of repositioning error (Angulation: Crown mesial/Crown distal; Vertical: Bracket occlusal/Bracket gingival; Rotation: Bracket mesial/Bracket distal; Combination of these).
10. Think about your cinch.
I typically cinch wires but vary the distance from the terminus of the tube to the beginning of the cinch based on the arch lengthening that I think I require. I tend to do this as I don’t like the idea of wire emerging horizontally from the molar tube and without cinching there is more risk of disengagement.
It is important, however, that the direction of the cinch does not impede tooth movement. I will therefore consider the anatomy may cinch vertically or lingually distal to the terminal molar. I use a mosquito ‘off-label’ (up to 0.018-inch NiTi) to do this as I dislike the hassle of annealing wires and find that wires are invariably ‘over-annealed’, compromising their physical properties, including shape memory.
So, these are my 10 Top Tips on Initial Alignment. Alas, the word count has gotten a little high!
Anyway, I hope you find these useful. Even if you don’t agree with some of the above, I hope these tips make you think a little more about your wire selection and engagement.
We would love to hear your thoughts, comments, and alternative approaches.

Professor of Orthodontics, Trinity College Dublin, The University of Dublin, Ireland
In tip no.2, “what are you objectives”, what do you mean by LA point?
regards,
chris
This is an excellent summary and very well thought out. I agree that early and frequent bracket repositioning and complete engagement of wires are two important keys to achieving the most ideal alignment as rapidly as possible.
What are you thoughts on using open coil spring to make space for a crowded tooth (teeth) vs using a smaller wire and engaging them even if they are short of space?
Thank you so much for this post🙏🏽. Could you elaborate on the mosquito off label? Is it a type of artery forceps Prof? I sometimes struggle with the size of the cinching plier head so I would love to try your way.