Bone anchored RME increases nasal airflow: A good randomised trial!
It is about time that I posted about a trial. This new study looked at the effects of bone anchored RME appliances on the airway. I thought that it was great.
The original RME devices were tooth borne and this resulted in the forces being applied to the maxilla via the teeth. A recent development has been the use of mini implants in the palate to anchor RME appliances. The force is applied directly to the maxillary bones. In theory, this reduces the effects of dental and alveolar bone tipping. This means that these new devices may have a greater skeletal effect and achieve greater airway change than tooth borne RME appliances.
A team from Orebro, Sweden and Homburg, Germany did this study. The EJO published it.
Farhan Bazargani , Anders Magnuson and Björn Ludwig
European Journal of Orthodontics, 2017, 1–4 doi:10.1093/ejo/cjx081
Unfortunately, this paper is behind the EJO paywall and only members of the EOS can get easy access to it. I wonder if they could think about making this open access?
What did they ask?
They did a simple study to ask a simple question;
“Does the use of a tooth borne RME (TB) or tooth-bone-borne RME (TBB) influence nasal airflow and nasal resistance in growing children with a constricted maxilla?”
What did they do?
They did a randomised controlled trial. The PICO was
Participants: 40 children aged 8-13 with uni or bilateral cross bite with a constricted maxilla
Intervention: A tooth borne RME device (TB)
Comparison: A tooth-bone borne RME (TBB)
Outcome: Rhinomanometric measured nasal airflow and nasal resistance before and after expansion. They also measured dental movement.
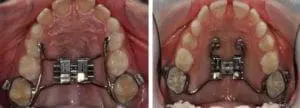
I thought that it was great to see that they did not get bogged down in a cephalometric and airway volume festival with multiple testing in the endless search for significance. Instead, they simply measure the effect of the treatment on nasal airflow etc. This is a good outcome measure as it is what counts and is relevant to the patients.
I thought that randomisation and allocation concealment was good. They recorded all the data blind including the airflow data. The statistical analysis was appropriate
What did they find?
They completed the trial and recruited 40 participants. Unfortunately, 4 of the TB and 6 of the TBB did not complete the study. This resulted in the numbers of drop outs in the two groups being unequal and means that there is some bias in the study. The authors addressed this, to a degree, by imputing data for the drop outs.
Their findings were clinically relevant. In brief, they found that there were no difference between the groups at the start of treatment. After expansion there was higher nasal flow in the TBB group with a mean difference of 51.0 cm3/s (95% CI 9.6-92.5). Similarly, there was a greater reduction in nasal airway resistance for the TBB group with a mean difference of -0.21 Pa s/sm3.
In summary, they did not find any differences in the dental movements. However, the TBB RME resulted in a significantly increased nasal airflow and decreased nasal resistance.
They pointed out that amount of decrease in nasal resistance was equivalent to the decongestive effect of a nose spray. As a result, this is clinically significant.
Finally, in their discussion, they felt that the TBB was more effective because the forces were delivered directly to the maxilla and not via the teeth.
Their conclusion was;
“When it comes to treating patients with constricted maxilla and upper airway obstruction, it might be wise to use the TBB RME instead of the conventional design. This could be more beneficial to the patient”.
What did I think?
I thought that this was an interesting study. The authors carried it out well and they reported it very clearly. They also dealt with the issue of “drop outs” using acceptable methods. It was also good to see that they addressed clinical and statistical significance.
This study adds to the data on the effectiveness of RME on the nasal airway. It certainly appears that the use of bone anchored RME is clinically effective.
However, before the “orthodontic airway physicians” and myofunctional orthodontists get too excited. We need to remember that this was a skeletally anchored RME device. We still know nothing about removable, semi-fixed or other magical devices.

Emeritus Professor of Orthodontics, University of Manchester, UK.
Would this have a chance to work on adults as well?
Dr. O’Brien..you make the job of reading between the lines and interpreting it so interesting. Very nice analysis and very tongue in cheek ending of the blog.I always wait for your blogs.Thanks for writing so well everytime.
Thank you for posting this interesting article. I wasn’t able to access the full text of the paper. How did the authors determine when to stop expansion? Generally, the end point is when the upper palatal cusps contact the lower buccal cusps (so as to avoid buccal cross-bite). The authors report no difference in dental movements. However, since this is tooth and bone borne, it is conceivable that a completely bone borne expander might lead to less tipping, greater sutural expansion and increase in nasal airflow…
Sounds interesting but the big question here is does it have a long term effect? For how long can we expect to get this nasal decongestant effect? Hasn’t it been shown that the skeletal effects of RME decrease with time?
how can we diagnose airway obstruction that is caused by a skeletal element and not caused by any other soft tissue element ?
because this treatment will be effective only if the patient has airway obstruction due to narrow maxilla and not due to any other obstructing factor.
thank you very much for this interesting study review
Without having read the paper (and I want too), as the dental movements were the same but one was partly bone-borne you would expect more skeletal expansion in the TBB group. It would be interesting to see if the TBB group had more turns to achieve the same dental expansion or more? If more, would a tooth-borne rpe given the same number of turns then achieve the same reduction in nasal resistance? Finally, do these changes in airway measures hold up over time (so I would love to see a follow-up to this study down the track. Congrats to the authors tho as we need this type of study.
Thanks Kevin.
Another question would be the longer term consequences if any or airway? Are these noted changes transient? These are truly significant as yet unanswered questions.
I like the idea of this study, however I have an issue with the the length of time between recordings. As they did 0.5mm turn a day, and completed the recordings immediately post retention, I would assume that the time difference being a maximum of 2-3 weeks at most. The literature has shown that the expansion relapses to a significant degree and that the airway volume/airflow/resistance also decreases post expansion. An additional query is also how there was such a large drop out rate considering the short time frame..
Hopefully the authors will be able to show some data with long term follow-up to better reflect the clinical situation.
There have been similar studies in adults, Mihai. Those studies were also published in a European journal. Those studies showed detrimental effects on the midface in adults. Our studies did not measure nasal airflow or nasal resistance, but using non-surgical protocols and biomimetic devices, we were able to increase both the midfacial skeletal volume (1) and nasal airway volume (2) in adults. The study that Kevin has kindly posted does not have a control group. So it’s impossible to decompose the effects of treatment and natural, nasopharyngeal growth that occurs in active growing 8-13 yrs olds. However, I agree with Kevin that most of the “magick” lies in the protocol. In that respect, ‘biomimetic’ devices attempt to harness the circadian rhythm(3).
1. Singh GD, Heit T, Preble D, Chandrashekhar R. Changes in 3D nasal cavity volume after biomimetic oral appliance therapy in adults. Cranio 34(1):6-12, 2016. doi: 10.1179/2151090315Y.0000000001. Epub 2015 Jan 27.
2. Singh GD, Heit T, Preble D. Changes in 3D midfacial parameters after biomimetic oral appliance therapy in adults. J Ind Orthod Soc. 48(2), 104-108, 2014.
3. Proffit WR, Frazier-Bowers SA.Mechanism and control of tooth eruption: overview and clinical implications. Orthod Craniofac Res. 2009 May;12(2):59-66. doi:10.1111/j.1601-6343.2009.01438.x.
Prof. Dave Singh, what were the detrimental effects of the midface in adults from RME? I was considering this as potential treatment for me in the future so it would be great to get more info on it…
Many Thanks
Do you mean procedures like MSE??