Breathe, breathe in the air: Part 3 Does orthodontic treatment cure childhood breathing problems?
Breathe, breathe in the air: Does orthodontic treatment cure childhood breathing problems?
This is the third and final part of my series on childhood sleep-disordered breathing and orthodontics and is about the effects of orthodontic treatment.
In the first post of this series, we concluded that the first line of treatment for children with disordered sleep breathing was tonsillectomy and adenoidectomy. Positive airway pressure could also be considered, but there are co-operation difficulties with this treatment. However, some practitioners suggest that orthodontic treatment has a role to play. As a result, I decided to investigate this issue. I think that this a controversial post!
I started by carrying out a standard computerised literature search. Unfortunately, I did not find any studies that had sufficient sample sizes or clearly defined questions to help me. Then I came across two systematic reviews, which I hoped would be able to provide me with a high level of evidence. I am basing this post on my interpretation of these reviews. Finally, I will try to draw some conclusions about childhood sleep-disordered breathing and orthodontic treatment.
Sleep Medicine Reviews published this systematic review;
Huynh et al
Sleep Medicine Reviews 25 (2016) 84e94
The authors aimed to investigate the efficacy of orthopaedic mandibular advancement and/or rapid maxillary expansion for treating pediatric obstructive sleep apnea.
They carried out a standard systematic review of the literature and included randomised trials and non-randomised studies. They found one RCT and one non-randomised trial that had evaluated the effect of advancement appliances. When they looked at RME, they found 2 RCTs and 3 non-randomised trials.
Whenever I read a systematic review, I have a close look at the papers that are selected. I found it very disappointing that when I read the randomised controlled trials, one was not an RCT (it was a retrospective cohort study) one was a small-scale feasibility study, and one was full of bias, lack of blinding, selective reporting and absence of essential data. So, I moved on to look at the other systematic review, which was in the Cochrane Library.
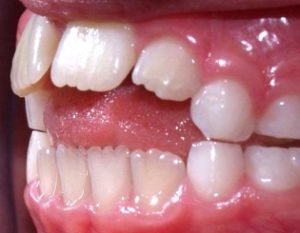 Orthodontic and orthopaedic treatment for anterior open bite in children
Orthodontic and orthopaedic treatment for anterior open bite in children
Cochrane Database of Systematic Reviews 2014, Issue 9.
DOI: 10.1002/14651858.CD005515.pub3.
This was a Cochrane review, as I have described before, these are very rigorous reviews and only include high-quality trials. They aimed to evaluate the effect of orthodontic treatment on anterior open bite and determine if there was an association between AOB, its treatment and sleep-disordered breathing. They found three RCTs that evaluated
- The effect of the Frankel 4 appliance and lip exercises vs control
- Repelling magnets vs bite blocks
- Removable appliance with high pull headgear vs control
They found that all three studies had significant problems with and were at high risk of bias concerning randomisation, concealment, blinding and they did not take sucking habits into account.
They concluded that recommendations on treatment could not be made from these studies.
So, the mainstream literature could not really help me answer the question on the effectiveness of orthodontic treatment on childhood breathing problems.
I then went to look at any evidence I could find about other methods of treatment, for example, myofunctional appliances, orthotropic and other methods. All I could see was simple poorly presented case reports in journals and websites……..I have discussed this previously.
I can only conclude that there is no or minimal research evidence that supports the use of orthodontic treatment as part of the treatment of sleep disordered breathing in children. I may have missed something here, perhaps someone can point me in the right direction and let me know if I missed something?
So what can I conclude?
When I started on this series of posts, I was optimistic that I would have found something positive to say about the role of facial growth and orthodontics and treating childhood breathing problems. I am very disappointed to come to these conclusions.
- Sleep-disordered breathing appears to be a significant problem for a proportion of children.
- The first line of treatment appears is the removal of enlarged adenoids and tonsils.
- There is very weak evidence that mode of breathing influences facial growth and skeletal pattern.
- There is very weak evidence that orthodontic treatment has a role in treating sleep disordered breathing.
However, this is a growth area in orthodontics, with active promotion of orthodontic treatment in treating SDB. Indeed, since I started this series, I have been exposed to degrees of patronising abuse on web pages, had posts removed and generally been made to feel uncomfortable for even trying to address this subject. This has been an interesting experience, and I suppose that I have been around long enough to make these suggestions.
- This area should be researched with randomised trials of interventions
- These studies will attract grant income because this is an important area
- If I were a young aspiring academic orthodontist, I would make this a primary focus of my work
- Can someone please do these studies?
If you are promoting orthodontic treatment to treat SDB, it would be great if you could
- Provide your patients, and the whole orthodontic community, with evidence on the effectiveness of the treatment that you provide. This is your ethical responsibility.
- If you are convinced that your own particular treatment is effective, engage with the research community and try to do some studies.
- Do not merely dismiss people, who ask questions, as being out of touch.
- Learn to critically appraise the literature and realise that a series of pictures on a website is not sufficient evidence to justify treatment.
Does this influence my practice?
Finally, since I did my speciality training, I always believed that mouth breathing influenced facial growth in severe cases and that I could help with breathing problems by expanding palates with RME etc. But the research that I have carried out to do this blog makes me very uncertain that this approach is supported by scientific evidence.
I work as an orthodontist in a Children’s Hospital and see children who have sleep-disordered breathing referred from my ENT colleagues. So what do I do the next time I see a drowsy looking child with a long face and bags under their eyes? I will modify my approach towards consent and explain that my treatment will be directed at correcting their malocclusion and if we get an improvement in breathing this will be a bonus. I certainly will not be informing them that I am carrying out treatment to improve their breathing. I can still sleep at night.
So that is breathing and orthodontics……just tumbleweed blowing down empty streets…
Comments are always welcome on my posts, so please make them!

Emeritus Professor of Orthodontics, University of Manchester, UK.
Another great post. Thanks. This is extremely informative for GDPs too.
If the evidence is lacking in terms of orthodontic treatment, but links between malocclusion and breathing disorders are shown, would you expect the extra emphasis on sleep disordered breathing recently to allow earlier detection, diagnosis and ENT treatment, leading to reduced severity of orthodontic problems? In other words, instead of orthodontic treatment helping, orthodontic diagnosis is helping.
Dear Kevin and Frank,
Informative as always and it is important to know what we dont know as what we do.
On Franks point, I looked at this recently and could find almost no good evidence on dental screening signs such as orthodontics for OSA.
Is there any good evidence for crowding per say rather than airway size? or Class II relationship rather than micrognathia?
Thank you,
Paul
Dear Prof. O’Brien
Thanks for your review. What you mentioned about your own previous ‘hunch’ (“…I always believed that mouth breathing influenced facial growth….and that I could help with breathing problems by expanding palates with RMR etc.”), while seemingly contrary to your previous admonitions of colleagues who might recommend/provide dentofacial orthopedic treatment options that are unsupported by robust evidence, I found it refreshing that at least at the beginning of your career you were so bold. And I completely agree with you that more data-driven efforts are needed; but I would add that such efforts should not be limited to Orthodontic departments working alone/ isolated, but also collaboratively include Pediatric Dentistry, Pediatric Medicine, Peds. Otolaryngology, Peds Sleep Medicine, Child Psychology departments in cross-disciplinary and multi-centered investigations. I’d also recommend you research the frequency of recurrent apnea post-T and A surgery, and also the mid-facial impaction effect of CPAP masks on pediatric patients. And finally Dr. O’Brien, what you mentioned about assuring that your informed consent is clear regarding what you as an orthodontist can actually offer a patient (expanded palate), to do, or have done otherwise (i.e., mitigate or cure apnea, etc.) would be/ would have been, both unethical and illegal (practicing medicine without a medical degree). I would encourage anyone who cares for children to at least assess sleep-airway hygiene as early in life as is feasible for you and make appropriate referral p.r.n. Ron Chervin’s scientifically validated Peds Sleep Questionnaire (PSQ) is downloadable for free from U Michigan website ….please use it!
Dr. O’Brien,
My latest Passion(not obsession yet) is identifying kids with SA type symptoms with Large Tonsils and have been convicted of being ADHD. I have been doing it for a while and with good success. Recently I have started to try to keep track of the kids that actually follow thru and get their tonsils removed. Pediatricians are the stumbling block. But, if I can get them past the pediatricians to the ENT, all goes well.
Now that you have caught my attention I will start keeping track. I use a subjective form filled out by the parent to screen the patients for SA. It seems to work quite well.
Dr. O’Brien-
Check out this article:
TREATMENT OF PEDIATRIC OBSTRUCTIVE SLEEP APNEA WITH ORAL APPLIANCES by Maria Pia Villa
M.P. Villa
Pediatric Clinic
Sant’Andrea Hospital
Via Grottarossa 1035/1039 – 00189
Rome, Italy
E-mail
[email protected]
Thanks, I looked at this paper very closely and I thought that it had many problems, for example, lack of clarity of randomisation, doubtful blinding, no allocation concealment and selective reporting of data. As a result, if I used any of the tools that measured bias, this study would be classified as high risk. The sample size was also very small and there was a high drop out rate. It was a good pilot study that could easily be improved upon, but it does not provide us with much other information
Dr. O’Brien – Not sure if you have reviewed these papers re: RME and OSA. One of them was a meta-analysis
PubMed PMID: 27031063, 26141004, 25934539, 24286909.
Hi and thanks for the comments. Yes, I did come across them and I decided not to include them in my post. The systematic review did not contain any trials and the other papers were all prospective cohorts with no controls. This is important because we need to remember that OSA has a natural history and some cases resolve with time.
Again I think that the focus should be in screen for and if appropriate refer patients that may benefit from a multidisciplinary assessment of a potential significant paediatric sleep breathing problem. We can identify some potential “diseased” individuals. This in itself will be great service to our patients.
The fact that some low evidence level articles with high risk of bias suggest some improvement in very specific sleep cycle parameters should not be considered a proof that treatment approaches such as maxillary expansion or mandibular reposition among children “cure” paediatric sleep breathing disorders. As mentioned before informed consent is not necessarily fulfilled if it is implied that those treatment approaches will consistently improve their signs and symptoms. It has to also be noted that the studied samples are usually 5-6 year old children. Those are not the usual ages when orthodontists or dentists with interest in orthodontics do maxillary expansion or mandibular reposition. Finally, it would be interesting to hear the hypothesis about how such treatment approaches do produce physiologic changes. There is a lot more discussion about what happens compared to why and how? This is maybe why we are stuck where we are by asking the wrong questions. Some food for thought.
Kevin:
I don’t think that this is a controversial post – but this might seem like a controversial reply, which I know you will take in good humor –
I agree there is very weak evidence that orthodontic treatment has a role in treating sleep disordered breathing. The reason in my mind is clear: airway deficiencies are not ‘orthodontic’ problems per se. Orthodontists are, typically, excellent at dento-alveolar mechanics, but once you get past those confines, the oral and maxillofacial surgeons appear on the horizon e.g. in anterior open bite cases, severe Class III cases and ‘gummy smiles’ inter alia. This leads me to suspect that a new specialty in Dental Sleep Medicine is required to target therapy at the site of interest i.e the upper airway (in both pediatric and adult cases). My experience in a cleft lip/palate team gives me the impetus to see in that direction. We have just begun some initial work to formulate a possible curriculum that might meet those requirements at some point in the future.
(Side note: Since I started my train of thought on how OSA might be potentially cured in adult cases, I have also been exposed to patronizing abuse, and generally been made to feel uncomfortable for trying to address this subject, by some of my orthodontic colleagues).
I also agree that OSA has a natural history – it’s called death. Please read about the recent demise of the late US Supreme Court Justice, Antonin Scalia. However, if we start early enough I believe that some chronic conditions, such as cardiovascular diseases, hypertension, diabetes, stroke and cancer can be mitigated, prevented and in some cases resolved.
I have not seen any evidence that some cases of OSA resolve with time. Please provide some pointers to the articles that support that contention. Thank you again –
Re OSA resolving without intervention…
Have a look at the papers published from the CHAT trial.
Hi Dave, thanks for the useful comments. How about leading some trials on this important issue? I mentioned in my first post on this series that systematic reviews have shown that OSA does resolve spontaneously. http://kevinobrienorthoblog.com/breath-breath-air-dont-afraid-care-sleep-disordered-breathing-orthodontic-treatment-part-1/
The way science works, is that any claims of prevention need to be substantiated by incidence/prevalence data and control groups. For instance, premolar extractions can prevent multiple sclerosis, glaucoma and amyloidosis. Please provide some data that disproves this contention.
Interesting to follow the debate. Lack of evidence is however, only telling us that we don’t know, not that the procedures are wrong or inefficient. I fully agree on your proposal that we need good studies on breathing problems but also on the role of myofunction and dentofacial development. Just looking on the picture you presented above from the article of Lentini-Oliveira et al makes you think that something caused this situation and it would be a good thing if we were able to prevent or reverse this unfortunate bite development at an early stage, the earlier the better. I also believe that cephalometric analysis that was used in the old studies (Linder-Aronson etc.) will not help us answering these questions.
Kevin, This is not directly related, but I am intrigued by the concept of facial growth and mouth breathing. I understand that there is a common belief that mouth breathing leads to a drop in the mandible and a low tongue position and a narrow maxilla and an anterior open bite, long face…..basically what has been called, “adenoid facies”. I have looked before and I haven’t found a long-term study showing this to be true, but it seems to be held as a common “truth”. So, my question has multiple parts: 1. As someone much more versed in the literature, is there such a study (or studies) that shows this to be true, 2. If so, should we be concerned when there is mouth-breathing and should we strive to obtain nasal-breathing? and 3. If it is true, shouldn’t we also be concerned with kids with ankyloglossia, because they cannot put the tongue in the roof of the mouth and wouldn’t we expect the same issues? 4. If #3 were true, would we need a longitudinal study to determine whether to proceed or would the reasoning that aberrant tongue posture causes aberrant growth, therefore, normalizing tongue anatomy to allow normal tongue posture (followed by possible myofunctional therapy to retrain) would be enough to decide this is a reasonable approach.
In response to question 3, there was a study published this year that links shortened lingual frenulum untreated at birth with obstructive sleep apnoea at a later age through it’s impact on tongue posture/function and orofacial growth. http://openres.ersjournals.com/content/2/3/00043-2016
I am one of those crazed orthodontists using passive self ligation. My goal is to treat without extractions as we gently expand the arches, although extractions are sometimes required of course.
I believe we can only improve breathing by broadening the arches – we’re not going to make it worse, but I too am cautious about over-promising. The improvement may be noticeable or significant, but perhaps not. No promises on that score.
I am currently treating a woman who is now off her CPAP machine and sleeping much better. Her physician and a sleep clinic are following that. I am but a humble orthodontist who (I hope) recognizes my limitations. I told her I was going to straighten her teeth, expand her arches and maybe breathing will be easier.
Breathing problems? One word – diet. Kids today eat scads of junk. Many kids and many adults too are walking containers of inflammation and edema. Soft tissue inflammation is a huge issue and it impacts breathing. And that same inflammation and the breathing issues likely impacts growth turning borderline vertical growers into ones with major issues.
Do I lecture my patients on this stuff? Nope. I don’t try to empty the ocean with a teaspoon either. We bug our patients enough on tooth brushing and oral hygiene. I’m no nanny.
My own personal experience was that I snored for years – to the point I considered soft tissue surgery. But I balked and I understand now that the tissue grows back – makes sense to me.
Over nine years ago I switched my diet to largely paleo – low carb, “primitive” or ancestral diet. I lost weight – about 30 pounds and I have kept it off. My snoring? Gone. I know that it was the weight loss partially, but I believe it was largely inflammation. I have much less and of course less fluid retention on lower carb diet. Eat a big spaghetti dinner and try to get your rings off the next day. You have absorbed lots of fluid and expanded your soft tissues. Kids are doing this every day with the junk – largely carbohydrates that they consume every day. It’s a combination of soft tissue edema from fluid retention from over-consumption of carbohydrates and inflammation secondary to those poor diets.
And those soft tissue changes are driving functional and growth changes that worsen the situation. Melvin Moss anyone? Skeletal growth is secondary, compensatory and obligatory. I love remembering that from grad school. Thanks Dr. Hechter.
I will stop here, lest I sound too crazy. I agree with the thrust of this article. As orthodontists there is a limit to the role we can play in breathing issues, but we can certainly help in some cases. Unfortunately, prediction is hard – especially about the future – sorry just had to add that last bit.
Anecdotally? It’s the diet, stupid – with apologies to James Carville. And I say that with humility. I was eating junk too. My diet is now what I would call slacker paleo, but I very rarely snore – only after lots of carbs, or after a few glasses of wine with some carbs. I am convinced that my general level of inflammation is much reduced – my soft tissues seem less reactive. If you snore, I would highly recommend experimenting on yourself. You will find aches and pains magically disappear as well – generalized inflammation is a huge health risk – perhaps one of the biggest we face.
Cheers!
Hello Kevin:
Sorry for the tardy reply but I wanted to go back and review what you said in Part 1. I found a couple of anomalies in your recent-most reply on re-reading Part 1. The systematic reviews you noted did not, as far as I can tell, say that OSA is self-resolving. They talked about a specific sub-group of children with adenoidal hypertrophy. Two points from this:
1. I was talking about OSA more broadly i.e. in Adults when I said that the condition is not self-correcting.
2. Pediatric OSA, which I believe is the focus if your comments, is a bit of a different animal. For example, a child may present with bed-wetting rather than sleep issues and other children may have obesity that precipitates breathing/sleep issues, etc.
The other interesting point for me is that you mention “Sleep disordered breathing is a common condition with an estimated prevalence primary snoring in children ranging from 8 to 27% and obstructive sleep apnoea from 1 to 5%”. I agree with that statement but it contradicts the recent finding of Larsen et al., which showed a 10% prevalence of OSA in children treated orthodontically with or without premolar extractions. The authors correctly pointed out that there was no difference in the prevalence of OSA with or without premolar extractions. The problem that I have with these findings is that their finding of 10% in both groups increased the risk of pediatric OSA at least twice and up 10 times in an orthodontic pediatric population. The authors justified their findings by saying that a 10% prevalence in the orthodontic groups mirrors the prevalence in adults but, IMHO, don’t think that’s a fair comparison, if we accept the concept that OSA is not self-correcting adults. I am looking towards collaborative research opportunities with US university-hospitals.