Early Class II treatment. Part 2: Are we clinician scientists or barber surgeons?
Early Class II treatment. Part 2; Are we clinician scientists or barber surgeons?
This is the second part of my post from last week. This is concerned with our presentation at the early treatment point/counterpoint discussion at the AAO conference 2015.
Jonathan Sandler started our session by discussing further data from the systematic review. He also pointed out that while the data suggested that routine early treatment is not effective; it does not mean that early treatment is not indicated for any patient. There always will be patients whose problem is so severe and/or they are being teased so badly that treatment is clearly indicated. In these instances, clinical experience needs to combine with evidence and patient opinion. This led to my final sections which I shall outline below. He also raised the question that if we ignore the evidence then we need to consider if we are clinician scientists or simply barber surgeons?
Evidence-based dentistry
The evidence-based care movement in dentistry has become firmly established. Nevertheless, there is a common misinterpretation that treatment decisions should be based solely on scientific evidence. This is not the case and I have discussed this previously in this post.
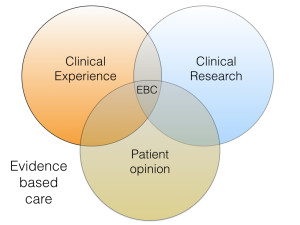
We need to remember that evidence based care has three main components and I have illustrated these in Figure 1. The best way to interpret this interaction is to consider that the initial stage of developing a treatment decision is based around a combination of evidence and clinical experience. This is then followed by the essential step of outlining the possible treatments to our patients, along with any available evidence. As a result, they are in a position to take an informed decision on their care. In a situation where there is substantial evidence, it is likely that the evidence will outweigh clinical experience, because uncertainty is reduced. However, when there is limited evidence clinical experience then carries more weight.
It is then clear to me that the most important component of this relationship is the information that we provide to our patients. If the evidence is high and uncertainty is low, we can provide evidence-based recommendations. We certainly cannot ignore the evidence and we should not be saying to them “there is substantial evidence that we should treat you in a certain way, but I’m going to ignore it completely because of my clinical experience”.
I would also like to point out that when evidence is lacking, there is nothing wrong with explaining to our patients that there is limited evidence, but our experience suggests that they should be treated in a certain way. Our patients will then have all the evidence required to make an informed decision as part of consent to treatment.
In the case of early class II treatment, the evidence is clear and we cannot ignore it if we are to ethically consent our patients to treatment.
Disappointment
 In my final comments, in our counterpoint, I expressed disappointment that we were having this debate. In this respect it is worth mentioning the comments of Dr David Sackett one of the founders of evidence-based medicine. In 1985 he spoke at the Moyers symposium and stated
In my final comments, in our counterpoint, I expressed disappointment that we were having this debate. In this respect it is worth mentioning the comments of Dr David Sackett one of the founders of evidence-based medicine. In 1985 he spoke at the Moyers symposium and stated
“Orthodontics is behind such treatment modalities as acupuncture, hypnosis, homoeopathy and on a par with Scientology”.
He then attended the Moyers symposium again in 1994 when the early results of the class II studies were being presented He responded by saying.
“All orthodontists should look with pride on these trials, for they mark the entry of your profession into the ranks of the scientific health disciplines”.
At this point the United States was leading in clinical trials. But since then I wonder if there has been a lack of momentum and researchers from other countries are beginning to lead the way?
Finally, at the end of our presentation, my overall feeling was disappointment that in the face of so much evidence we were still debating early class II treatment. Indeed, Drs Dugoni and Oh suggested that this was a controversial area! I propose that it is not; we have the evidence on this clinical question. It is time to move on… or indeed, are we clinician scientists or barber surgeons?

Emeritus Professor of Orthodontics, University of Manchester, UK.
I agree with you there are some severe cases that benefit from early treatment but the vast majority is based in greed. “If I can get some appliance on this kid then he’s mine and no one else can touch him& he’ll be mine for the second phase!”
It’s funny, the orthodontists who used to criticize me for limited early treatment of severe problems have now imbraced it with open arms like they just found God & religion.
Dentistry has become a get rich scheme instead of a career & a profession.
Hi Kevin.
Thank you, once again. I appreciate your clear and concise review of the relevant literature on this and other important orthodontic topics.
Are you familiar with any rct’s or reviews that address signs and/or symptoms of tmd when comparing severe class 2 control vs. treated patients using a combination of fixed orthodontic preceeded by removable appliances, Herbst, Forsus type appliances? Over the past several years, I have had orthodontists consult with me about the legal, including the nature and extent of informed consent, and ethical issues due to my background as an orthodontist, trial lawyer and former judge. I suspect that the issue will likely present more frequently in the future and would appreciate your assistance.
Thank you, as always.
Warmest regards,
Don Machen
Dear Dr. O’Brien,
While reading your article comparing treatment in one and two phases, I came accross this sentence: “Adolescent treatment is treatment provided in 1
stage carried out with functional or fixed appliances.”
I was wondering, just out of curiosity, if you compared your twin-block cases treated in phase 2 with an untreated control in terms of mandibular parameters, and what the results were. Now that accelaration rather than true mandibular growth seems to be the case, would it be unethical to run an RCT comparing class II patients treated with fixed appliances with another group receiving functional appliance during the peak followed by fixed appliances? If I am not mistaken, I remember that you once mentioned that this type of study had already been done. If yes, can you please provide me with the reference?
I am always running in circles around this possible RCT:
Part 1: Group 1 (functional) vs Group 2 (untreated Cl.II) during peak
Part 2: Both receive fixed appliances and are compared after peak.
Too much of a wheel reinvention? I know there’s a systematic review, but the evidence is low. Right?
Hi Fabio, thanks for the comments. We did not compare the twin block patients treated in phase 2 with an untreated control, as this would not be ethical. I think that it would be ethical to run a trial comparing Class II collection with fixed appliances and functional appliances. I do not think a trial has been run in this area.
I hope I’ve answered your questions?
Best wishes Kevin
Dear Prof O’Brien,
Thank you for interesting blogs about the pyramids of evidence and denial as well as evidence based dentistry in relation to early class II treatment.
I am by no means in a position to debate this topic as I lack the expertise and represent a more commercial (and thus biased) standpoint. Nevertheless, I would humbly like to raise two questions:
1. In the spirit of evidence based dentistry, RCTs should only be used as evidence within the relevant context. The results of an RCT made with certain inclusion criteria may or may not be generalisable to a patient outside of the inclusion criteria (age, ethnicity, severity etc). For example, if an RCT shows that treatment X is effective for a population of 10-15 year old patients, it might be risky to conclude that the same treatment is effective in 15-20 year olds or even in 14-15 year olds. Likewise, if there is an RCT showing that treatment Y is ineffective in a population of 15-20 year olds, it may or may not be true that the same treatment is ineffective for 10-15 year olds. Sometimes, the number of RCTs concerning a certain topic is limited and it may be tempting to extrapolate the results outside of the original context. Rawlins discusses the risks of generalizing RCT results in his Harveian Oration http://dx.doi.org/10.1016/S0140-6736(08)61930-3 or http://www.amcp.org/WorkArea/DownloadAsset.aspx?id=12451 ). In orthodontics the number of RCTs concerning a certain question is often rather limited. How can one know that the number of RCTs is sufficient to be sure that we have the evidence on a clinical question?
2. Meta-analyses are indisputably on the top of the pyramid of evidence. A meta-analysis can nevertheless only be as good as the RCTs (and NRSs) it is based on. The RCTs in the Cochrane review you refer to seem to show extreme heterogeneity as discussed by Schroll et al (http://dx.doi.org/10.1186/1471-2288-11-22 ). This heterogeneity may perhaps indicate that there were some differences between the RCTs that caused the outcomes to differ from each other. Doesn’t this suggest that there may still be something unknown that needs further research? In other words, are all early class II treatments equal or may some protocols be effective although others are not?
I apologize for being a bit provocative.
Respectfully,
Valter
P.S. I realize I’m on thin ice as my expertise in research methodology is very limited. If I have misunderstood something or made statements on incorrect or vague grounds, please disregards this comment and accept my humble apologies!
Hi Valter, Thanks for the message and you raise some really important points. If I deal with your initial point. Yes it is totally correct that you should not generalise the findings from trials and are not relevant in terms of age groups and morphological characteristics. This is why further trials are needed in orthodontics to answer the questions that are relevant to older age groups regarding Class II malocclusion.
there was a heterogeneity between the trials and this was particularly relevant with cephalometric analysis. this may be reduced by the adoption of core outcome sets for trials and we are currently looking at this for orthodontic treatment. I agree with you that that we do not know everything and further research is needed, however, these trials did look at the same question with similar methodology and came to similar conclusions. As a result, they do go some way to reducing uncertainty about this problem. I feel that there is no need to carry out further research this specific area but there are many other areas that do require further study.
I hope that I have answered your questions than you are not being provocative at all you are being very insightful!
Best wishes Kevin
I agree with Dr. Strole. This reminds me of the “engagement ring lingual holding arch”, placed around age 8 years, well before the E-space is available to capture the patient.
My definition of early treatment: any treatment performed before 8 a.m.
FYI: Dr. David Sackett passed away May 13, 2015.
http://fhs.mcmaster.ca/sackettsymposium/sackett_dave.html
Yes, this was a couple of days before our talk. I saw him lecture a couple of times, he was an inspiration.
Dear Dr. Kevin,
More clear is impossible! As you, I wish one day this kind of debate would not be necessary. Instead, we could debate new researches designs of clinical trials, systematic reviews in a way to find out new evidences where still there are lacks of evidence. The clinician’s scientists thank you for share your thoughts and wisdom.
Great note, congrats. Here in Mexico, or even in Latino America, is a tricky question “Are we clinician scientists or barber surgeons?” because a dentist usually think “I´m not a scientist, I´m not a barber… I´m an artist” that´s worse. Thank you so much for this post and your hard work for this blog. Kudos
Dr. O’Brien,
I thoroughly enjoy your blog. Thank you for your commitment to the specialty.
I’ve noticed that some of the other readers have made comments about early treatment in general. This is something that I embrace in my practice, while informing the patient and the parent that this is exclusively for esthetics and does not mean that they won’t need a comprehensive phase of orthodontic treatment in the future. My treatment plan involves light leveling the anterior teeth with a 2×4 and consolidation of space over a period of 6-8 months. I’ve never noticed any issues in my final records, but I have met some resistance from colleagues who claim that “moving teeth with open apices can cause damage” and aligning the upper laterals can “tip the root into the maxillary canine and cause root resorption.”
I’ve found some literature which showed that orthodontic treatment on teeth with open apices has a protective effect against root resorption (Magravani M. Changes in root length during orthodontic treatment: advantages for immature teeth. Eur J Orthod. 24 (2002) 91-97), but I have been unable to find any studies that evaluated potential root resorption of the maxillary lateral by the canine follicle during alignment.
I was hoping you could offer me some insight on this topic or perhaps make it a subject of a future blog.
Many thanks.
Kind regards,
Moonyoung Lee
Dear Dr Kevin O’Brien,
Congratulations, for sustaining such wonderful blog, In a court of law where the decision on malpractice is largely based on experience based practice, though there is change towards evidence based practice, how can a practitioner substantiate denial of treatment in children when risk of trauma to incisor and psychological advantage is better if treated early early. In Helling vs Carey two ophthalmologists were held liable for not routinely screening a patient for glaucoma, even though it was not the standard of care adopted at that time. The results of RCT / Systematic review is, (though generalization is not possible) is for a population or age group, but a case in court is always individual based. Thank you very much, keep going.
Thanks for the comment. This is a difficult point that you have raised, but I think that it can be addressed by consent. I inform my patients of the evidence or lack of evidence and then let them decide on whether they want to undergo treatment. The key is giving them all the information and not just my personal opinion. This is then carefully recorded in the notes. I think that this should keep me out of the courts!
Best wishes: Kevin
Dr Kevin,
I have recently started reading your blogs and I find them very useful.
Thank you very much.
On your blog on correction of class II malocclusion your conclusion is that only those who are at risk of trauma or being teased are the ones who shout be treated.
However we do come across a lot of class II malocclusion cases where functional appliances are the only choice of treatment.
We may not get lengthening of mandible but the dentoalveolar changes that we get are the only changes that you would eventually get. Also the vertical opening of mandible that we get without opening the mandibular angle can not be ignored. I feel you cannot get those results with fixed appliances.
I hope I have been able to convey my message and your very valuable views will be highly appreciated.
ORthodontics is not merely smile design and bite….but
….
“Orthodontics is behind such treatment modalities as acupuncture, hypnosis, homoeopathy and on a par with Scientology”.
What a great value addition . but the mainstream of orthodontists ignoring it ? Why ? Does this repeat the sony tv or kodak camera or nokia mobile story