Back to Basics 2: Predicting the pubertal growth spurt
This post is my second blog of a series on craniofacial growth. As in the previous post, I will revisit some of the basics.
Last week, we discussed jaw growth during the pubertal growth spurt and the evidence that peak height velocity is associated with increased mandibular growth. This week we will discuss methods aiming to predict the pubertal growth spurt.
Wouldn’t it be great to predict the pubertal growth spurt?
The ability to accurately predict the timing of the pubertal growth spurt is of interest to many specialities within medicine and surgery, not only orthodontists. Investigators have described many methods over the years.
We can broadly divide these into those that employ relatively simple non-invasive examination (chronological age, height-velocity or secondary sexual characteristics) and those that investigate the maturation of the skeleton or dentition using radiographs.
- Chronological age and peak growth velocity (standing height): can provide a guide to developmental status. However, they are generally poor predictors of a child’s maturational status, including the pubertal growth spurt. Longitudinal monitoring of height will be inaccurate in predicting the pubertal growth spurt by more than one year in a third of cases.
- Secondary sexual characteristics: such as the onset of menarche in females or voice changes in males have also been used. Unfortunately, they generally indicate that the growth spurt has already been entered or passed.
There appears to be a relatively limited predictive value associated with these non-invasive methods. As a result, some workers have suggested that skeletal or dental maturational staging from a radiographic examination may predict both the pubertal growth spurt and expected growth. These methods include hand-wrist radiography and cervical spine vertebrae analysis.
Hand–wrist radiographs:
The small bones of the hand and wrist go through a series of predictable and identifiable ossification events during skeletal development. We can view these using hand-wrist radiographs. Importantly, we can take these easily, see many bones within a small area, and use them to predict skeletal age and maturity. We may do this by either comparing them to population averages in a reference atlas; or by evaluating specific ossification events (ulna sesamoid, hook of the hamate middle phalanges).
However, while overall facial growth velocity and, to a lesser extent, maxillary and mandibular growth velocity are related to skeletal maturity and prediction of the pubertal growth spurt can be improved using hand-wrist radiographs, reliability is low. For these reasons, it should not be regarded as acceptable to take hand–wrist radiographs to predict future facial growth or the timing of the growth spurt.
Cervical Vertebral Maturation (CVM):
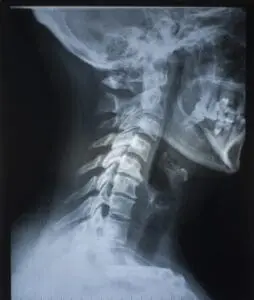
The cervical vertebrae undergo well-defined ossification changes. These correlate with different stages of hand–wrist development. Given that we can see the upper cervical vertebrae on a cephalometric radiograph, this precludes the need for additional radiation when undertaking this analysis. As a result, the CVM method is preferable to hand-wrist radiographs. Although, taking a cephalometric radiograph expressly to undertake or assess the progress of CVM is more difficult to justify.
This has led to research workers advocating that the CVM method can detect the onset of peak mandibular growth. Furthermore, as this correlates with maximal growth of the mandible, it may be logical to suggest that treatment with a functional appliance during this time period will result in increased mandibular growth.
CVM uses the morphology of the second (C2-odontoid process), third (C3) and fourth (C4) cervical vertebrae bodies to identify growth stages. This method is based on data from only 18 males and 12 females from the University of Michigan Longitudinal Growth Study.
Six stages of CVM
These authors also define six stages of maturation (CS1–6), which may predict future growth in subjects with mandibular deficiency. The chronological age corresponding to each CS stage has recently been systematically reviewed. I include the mean values and confidence intervals (CI) below. It appears that girls have earlier maturation than boys, and there is variation in skeletal maturational age between continents:
- CS1 or CS2[CS1: 9.7 (CI 9.4-10.1) years; CS2: 10.5 (CI 10.5-11.1) years] peak mandibular growth will occur on average either 2 years or 1 year after these stages, respectively (a concavity in C2 indicates that the growth spurt is approaching); the clinician can wait at least 1 year before considering functional appliance treatment;
- CS3[12 (CI 11.7-12.2) years] peak mandibular growth will be achieved within 1 year after this stage; it is, therefore, the ideal time to start functional appliance treatment;
- CS4[13.4 (CI 13.2-13.6) years] peak mandibular growth has been achieved within 1–2 years before this stage; and
- CS5 and CS6[CS5: 14.7 (CI 14.4-15.1) years; CS6: 15.8 (CI 15.3-16.3) years] are post-pubertal; peak mandibular growth has ended at least 1 or 2 years before these stages, respectively.
Evidence-based historical growth data suggest that we can expect the total mandibular length to increase an average of 5.4 mm in the year following CS3, compared to 2.5 mm between both CS1–2 and CS2–3; 1.6 mm between CS4–5 and 2.1 mm between CS5–6.
This seems very useful. However, the literature also contains several studies by Ball et al., Beit et al. and Mellion et al. that have failed to identify any significant correlation between the CVM stage and peak mandibular growth spurt. Furthermore, the diagnostic reliability of this technique has been questioned (Perinetti et al., 2018).
Dental development:
Development of the dentition based upon calcification stages derived from radiographic examination is also a potential method of predicting the pubertal growth spurt.
Importantly, it does not require additional radiographic exposure when conducted in conjunction with routine diagnostic radiography. Several detailed indices of dental calcification have been described by Moorrees and Demirjian.
Nevertheless, there is wide variation between the development of the dentition and chronological age. While Bittencourt and Baretto have identified correlations between dental development and skeletal maturation assessed from hand-wrist radiographs, this evidence is low with much heterogeneity. Unfortunately, an association with the pubertal growth spurt is not established..
Facial growth and indices of maturation
An interesting study by Lysle Johnston, published a decade ago, remains pertinent. This investigation utilised the Bolton-Brush Growth Study archive and investigated patterns of facial skeletal growth and their relationship to various standard indices of maturation (Mellion et al., 2013). They selected serial records of 100 children (50 males; 50 females) to encompass the onset and peak of the adolescent facial growth spurt, with chronological age, height, cephalometric and hand-wrist films available for most ages.
- For females, the onset of the pubertal growth spurt in height, facial size and mandibular length occurred at 9.3, 9.8 and 9.5 years, respectively; whilst the peak occurred at 10.9, 11.5 and 11.5 years;
- For males, the onset of the pubertal growth spurt in height, facial size and mandibular length occurred more or less simultaneously at 11.9, 12.0 and 11.9 years, respectively. Whilst peak in height occurred slightly earlier than the peaks in facial size and mandibular length at 14.0, 14.4 and 14.3 years;
- Regarding growth prediction, hand–wrist radiographs indicated that maturation had reached peak velocity. While chronological age was nearly as good, CVM was consistently the worst.
This study provides evidence that the onset and peak of the pubertal growth spurt do seem to occur in males ages 12 and 14 years. However, the assumption that the equivalent ages in females are 10 and 12 years seems to be six months to 1 year too late.
Next week, I will look at the evidence base about whether timing functional appliance treatment to coincide with the growth spurt does result in more mandibular growth…………………perhaps the most controversial subject!

Great review of literature. Why do you reference correlating treatment timing specifically with a functional appliance? It’s not like that appliance grows mandibles significantly more than other orthodontic treatments.
The improvement in PAR index after treatment with functional appliance has been attributed to the net correction produced by dentoalveolar and not significant skeletal changes produced by functional appliance.Moreover differential mandibular growth is not predictable. Mandibular differential growth has a complex relationship with the maxillary growth and molar eruption. Obviously the interpretation of improvement in PAR INDEX is crucial.
Thanks for a great review to help us keep up to date !!!