A brief guide to removable functional appliance treatment
A brief guide to removable functional appliance treatment.
Last weeks posting on removable functional appliances and the results of a recent systematic review attracted a lot of interest and was hit almost 1000 times a day. I also received more comments than any other post. These are worth reading. As a result, I have decided to postpone my next post on the evidence behind Acceledent and continue with the theme of functional appliances.
In view of the interest that was shown in this clinical area I think that this is a good time to consider an evidence based approach to Class II treatment. My colleague and friend Professor Jonathan Sandler has worked with me on this post. We will divide this up into several main areas and problems
Early treatment
As we all know, this type of treatment has been researched extensively and several trials and systematic reviews have been published. I have discussed these in previous blog posts on the results of systematic reviews and the incidence of incisal trauma. I have also discussed that the provision of care should be based on a combination of evidence and clinical knowledge in this post.
We think that the research evidence is very clear on most of the outcomes of treatment. In summary, early treatment, in addition to a later course of orthodontic treatment, compared to a single course of treatment in adolescence, does not have a more favourable influence on: the skeletal pattern, final occlusal result or the need for extractions.
Early treatment does however, lead to a transient increase in self-esteem and there is also weak evidence that it reduces the incidence of incisal trauma. One decision that we need to be make is whether the child’s self-esteem is in need of a boost at this stage or whether, bearing in mind the downside of doing two courses of treatment in terms of cost to the patient, the parent or the state, it would be better to wait until definitive treatment can be performed in one phase at a later stage.
When we consider the risk of trauma we need to evaluate if the child is at risk because of their general activities.
As a result, we feel that early treatment should not be routinely prescribed for patients with large overjets, but may be considered if one of our patients is either being harmed due to excessive teasing at school, or has a sufficiently large overjet (or lifestyle) that we feel makes them at a serious risk of significant trauma.
Patients in the late transitional or early permanent dentition with moderate overjets (6-10 mm) often with a moderate skeletal discrepancy.
We feel that, again, this decision is clear and we have a high level of certainty. We would tend to treat this group with a Twin Block. For the following certainties that are derived from our study into the effectiveness of Twin Blocks vs Herbst.
- There is a a rapid correction of the overjet in most patients
- Co-operation is reasonable, with a non-compliance rate of 30% in the UK.
- They are much less expensive than the Herbst appliances
- They are significantly easier to manage when problems occur
- The transition from the Twin Block to fixed is straightforward.
We know that this appliance will reduce the overjet, mostly by tipping of the teeth but it will not change the skeletal pattern to a clinically meaningful degree (although, occasionally we ‘strike lucky’ and see patients with very favourable mandibular growth). Importantly, we cannot predict those patients who are going to grow well and those whose teeth will purely tip.
We think that it is important that we inform patients that the evidence shows that their facial skeleton is not going to change significantly but we will certainly correct their appearance, if they co-operate with treatment.
Patients with a severe overjet and skeletal discrepancy.
This is where we have most uncertainty, and this is reflected in the comments that were made on the previous post. We are now faced with a genuine dilemma.
Do we…
- Treat them now with the main aim of reducing the overjet and the overbite with a combination of upper and lower incisor tooth movement and accept that this will leave the child with a (camouflaged) skeletal discrepancy.
- Avoid treating now and wait until the patient has stopped growing and then provide definitive orthognathic treatment to fully correct the overjet and overbite as well as the skeletal discrepancy.
If we consider these options:.
The advantage of option 1 is that we will correct the overjet, overbite and sometimes the transverse problem (Figure below). This improvement in dental appearance as well as the associated soft tissues, during the formative adolescent years, may have benefits in self-esteem (although research evidence is lacking). We could argue that as this is a critical time in a child’s life when they learn most of their interpersonal skills. With the possibility of improved appearance they maybe happy to accept that their skeletal discrepancy is still present albeit in a much less noticeable form.
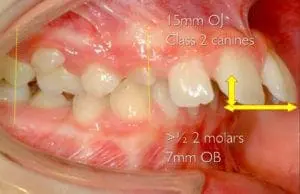
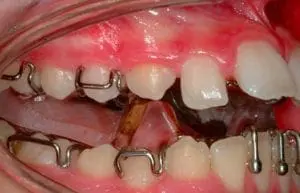

The disadvantage is that while we can attempt to correct the overjet, the patient may still be unhappy with their final facial appearance and they may request orthognathic surgery later. This will, mean undoing the dento-alveolar compensation that we achieved in our earlier course of treatment which might add an extra 6 months to the fixed appliance phase of treatment. Furthermore, in severe cases where camouflage is attempted we may run the risk of over proclination of the lower incisors and compromise gingival health.
The advantage of option 2 (surgery)is that we can correct both the dental and skeletal discrepancy in one course of treatment. Theoretically, there should be less uncertainty with this approach.
The disadvantage is that we will leave these impressionable teenagers during their formative years with a substantial malocclusion.
What is our solution?
Our feeling is that the solution to our dilemma involves explaining all of these uncertainties to the patient and their parents. This means that they will then be aware of all the risks and benefits of each approach to treatment. They can then play a very active role in reaching the important decision of how to proceed.
Other areas of uncertainty.
While we feel that we have outlined sensible approaches to these clinical problems, there are still some other uncertainties. One of these is whether using fixed appliances and some form of Class II mechanics, whether it is a fixed Class 2 corrector or headgear and class 2 elastics, will result in a similar result to a course of functional appliance therapy. As some people argue that functional appliance treatment is simply a method of applying Class II traction. Our feeling is that we do not know for certain and it may, therefore, be useful to carry out a trial in this area.
As things stand, we would prefer to use Twin Blocks, on most patients with large overjets, presenting in the early adolescence mostly because we are confident that we can achieve our desired result with a functional appliance providing the patient will cooperate with treatment.
Summary
In summary, we feel that the evidence for the treatment of Class II malocclusion is available and can be readily interpreted. This is a mixture of the “art and science’ of orthodontic care. It is important to remember however that despite being able to improve appearance significantly we just cannot grow mandibles!

Emeritus Professor of Orthodontics, University of Manchester, UK.
Realy helpful. Keep it up.
Well written by you and Jonathan – thank you.
Still leaves the question; why not just use class II elastics and not bother with a functional appliance?
Hi Dai, sorry we forgot that bit! If we accept that a Twin Block porcelains the lower and retroclines the upper incisor (and this is the evidence). Then Class II mechanics on fixed appliances should be effective. However, we feel that an effective method of achieving this change can be done by a Twin Block and this may be a simpler form of mechanics? But this is influenced by operator preference and skill.
The major weakness in all of this is the 30% non compliance rate with functional appliances.
This is not a reasonable failure rate. Whoever funds this treatment, be it the State, third party insurance or private sources begin a payment programme only to be told that nothing has been achieved. This can be some months into an intervention and thus the amount is not insignificant.
Fixed appliances under the same circumstances in achieving similar results fail at significantly lower levels.
Dear Kevin,
I liked very much this post. It is a great generosity from you and Dr. Sandler for the Orthodontic community.
I think this is a confident and trustful approach. However, I would like to make a comment about the certainty in your summary when you said, “we just cannot grow mandibles”. It is important to point out that this is our current evidence with our actual methodology.
Maybe new studies in different areas can change this evidence. So, I think is better to say, “we just cannot grow mandibles, till now”.
Dear Dr Kevin
I would like just to inform you that, since 2001, in France we use the PUL appliance, a light Herbst functional mandibular advancer, which has two advantages:
1- High rate of compliance (more than 90%) in young and teens patient who wear it 22 hour/24
2- It is customized for each patient.
You can have all information on the website: wwwpulconcept.com
Regards
How long would you use the functional appliance for?
The functional appliance phase in our studies was about 12 months, then the fixed was approx 12 months. If I am not getting any reduction in oj change after 3-4 months, I stop treatment with the functional and consider other methods of treatment
Dr. Obie, maximal jumping or stepwise advancement?
Dear Kevin
I would like to reply to Klaus Barretto Lopes comment. We can’t grow mandibles but we can reposition them forward – Form follows Function – and then the whole TMJ complex remodels. Anyway, that is my experience in almost 30 years of orthodontic practice.
Dear Helen:
I would be very interested to hear why you conclude that the TMJ complex remodels after the mandible is re-positioned forward. My conclusion, after nearly 25 years of trying to grow mandibles, is just the opposite: the condyle remains re-positioned and out of the fossae. I don’t think that our particular appliance choices (I have used many) is sufficient to explain our differing conclusions. What do you think?
Delighted to have stumbled upon your blog Kevin. Your posts are indeed thought provoking.
I would like to ask what you think about ‘repositioning the mandible forward’ as Helen points out. Would you know of any relevant studies that focus on the long term effect and treatment of the ‘foot and shoe principle’ wherein the mandible is ‘locked’ into a narrow maxilla? Do you prefer to initiate an early treatment as a form of interception in such cases?
Helen, would be great to hear your experience on such cases as well!
Hi Rohit
Apologies for the late reply but I have been away. In my experience development in the maxilla in both the lateral and sagittal planes will result in spontaneous repositioning of the mandible when carried out in the mixed dentition. An upper anterior inclined bite plane can also be helpful. In some cases a Bionator, Bioblc stage 3 or 4 and other similar appliances will be required. In my opinion the Twin Block is not as beneficial because of the reciprocal forces on the maxilla.
Dr Paul Coceancig of Newcastle, Australia has a graphic 3D video of the changes that take place with the Hirax appliance and the IMDO technique. You can find this on his YouTube site. As a surgeon he favours the IMDO surgical technique but functional orthodontists favour the appliances that I have already mentioned. His imaging shows very clearly the benefit to the airway that maxillary development and mandibular correction can achieve.
Kevin: I am new to your website/blog. ally great information.
If we agree that nobody can grow the mandible and it is difficult to distally drive upper molars, when we use functional appliances, are we just moving the lower teeth forward? and does bone get deposited on the labial of the roots of the lower incisors? or the bone does follow the roots of the lower incisors? I would like to know your opinion.
thanks
Rob
Hi Rob, you are correct. Most prospective research has shown that all functional appliances procline the lower incisors. There has also been work done by Pancherz that showed that this proclination does not do harm and that the alveolar bone remodels.
Hi Kevin. I would like to ask if there is any related articles showing the significance of lip incompetence in the treatment planning of Class II div I malocclusion? Thank you.
If Functional appliances work by tipping the teeth, how do you explain the change in molar relationship towards class I (just natural forward growth?, i.e. would it have happened anyway.) Some people say there is an element of posture, but if this is the case my patients wouldn’t be able posture 8-10mm further forwards than their new ‘postured’ edge to edge position post functional. Please can you explain how the functional appliance helps the molar relationship to change if its not growing mandibles and if its not posture?
condyle-fossa relationship