A sensible guide to removable functional appliance treatment?
This weeks post is a summary of the evidence behind the use of removable functional appliances. It is an update of an earlier post in 2014.
I am just back from the AAO meeting in Los Angeles. At this meeting, I saw several presentations on the use of growth modification appliances. As usual, presenters made claims about growing mandibles and improving breathing. As a result, I thought that it would be a good time to revisit some of the basic information on the correction of Class II problems with removable functional appliances. I am also massively jetlagged and I cannot write a new post today!
I published the original post on this method of treatment in December 2014.
My colleague and friend Professor Jonathan Sandler worked with me on this post. We will divide this up into several main areas.
Early treatment
As we all know, this type of therapy has been researched extensively, and several trials and systematic reviews have been published. I have discussed these in previous blog posts on the results of systematic reviews and the incidence of incisal trauma. I have also explained that the provision of care should be based on a combination of evidence and clinical knowledge in this post.
We think that the research evidence is unequivocal on most of the outcomes of treatment. In summary, early treatment, in addition to a later course of orthodontic treatment, compared to a single course of treatment in adolescence, does not have a more favourable influence on the skeletal pattern, final occlusal result or the need for extractions.
Early treatment does, however, lead to a transient increase in self-esteem and there is also evidence that it reduces the incidence of incisal trauma.
We, therefore, need to make an important decision on whether the child’s self-esteem requires a boost at this stage or if it would be better to wait until definitive treatment can be performed in one phase at a later stage.
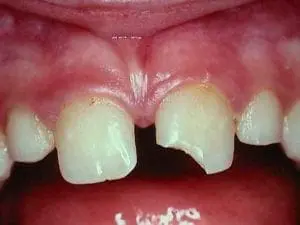
When we consider the risk of trauma, we need to evaluate if the child is at risk because of their general activities.
As a result, we feel that early treatment should not be routinely prescribed for patients with large overjets, but may be considered if one of our patients is either being harmed due to excessive teasing at school or has a sufficiently large overjet (or lifestyle) that may put them at risk of significant trauma.
Patients in the late transitional or early permanent dentition with moderate overjets (6-10 mm) often with a moderate skeletal discrepancy.
We feel that, again, this decision is clear and we have a high level of certainty. We would tend to treat this group with a Twin Block. For the following certainties that are derived from our study into the effectiveness of Twin Blocks vs Herbst.
- There is rapid correction of the overjet in most patients
- Co-operation is reasonable, with a non-compliance rate of 30% in the UK.
- They are much less expensive than the Herbst appliances
- They are significantly easier to manage when problems occur
- The transition from the Twin Block to fixed is straightforward.
We know that this appliance will reduce the overjet, mostly by tipping of the teeth but it will not change the skeletal pattern to a clinically significant degree (although, occasionally we ‘strike lucky’ and see patients with very favourable mandibular growth). Importantly, we cannot predict those patients who are going to grow well and those whose teeth will purely tip.
We think that it is essential that we inform patients that the evidence shows that their facial skeleton is not going to change significantly, but we will undoubtedly correct their appearance if they cooperate with treatment.
Patients with severe overjet and skeletal discrepancy.
This is where we have the most uncertainty, and this is reflected in the comments that were made on the previous post. We are now faced with a genuine dilemma.
Do we…
- Treat them now with the main aim of reducing the overjet and the overbite with a combination of upper and lower incisor tooth movement and accept that this will leave the child with a (camouflaged) skeletal discrepancy.
- Avoid treating now and wait until the patient has stopped growing and then provide definitive orthognathic treatment to adequately correct the overjet and overbite as well as the skeletal discrepancy.
If we consider these options:.
The advantage of option 1 is that we will correct the overjet, overbite and sometimes the transverse problem. This improvement in dental appearance as well as the associated soft tissues, during the formative adolescent years, may have benefits in self-esteem (although research evidence is lacking). We could argue that as this is a critical time in a child’s life when they learn most of their interpersonal skills. With the possibility of improved appearance, they may be happy to accept that their skeletal discrepancy is still present albeit in a much less noticeable form.
The disadvantage is that while we can attempt to correct the overjet, the patient may still be unhappy with their final facial appearance and they may request orthognathic surgery later. This means undoing the dento-alveolar compensation that we achieved in our earlier course of treatment which might add an extra 6 months to the fixed appliance phase of treatment. Furthermore, in severe cases where camouflage is attempted, we may run the risk of over proclination of the lower incisors and compromise gingival health.
The advantage of option 2 (surgery)is that we can correct both the dental and skeletal discrepancy in one course of treatment. Theoretically, there should be less uncertainty with this approach.
The disadvantage is that we will leave these impressionable teenagers during their formative years with a substantial malocclusion.
What is our solution?
Our feeling is that the solution to our dilemma involves explaining all of these uncertainties to the patient and their parents. This means that they will then be aware of all the risks and benefits of each approach to treatment. They can then play a very active role in reaching the critical decision of how to proceed.
Other areas of uncertainty.
While we feel that we have outlined sensible approaches to these clinical problems, there are still some other uncertainties. One of these is whether using fixed appliances and some form of Class II mechanics, whether it is a fixed Class 2 corrector or headgear and class 2 elastics, will result in a similar result to a course of functional appliance therapy. Some people argue that functional appliance treatment is simply a method of applying Class II traction. Our feeling is that we do not know for sure and it may, therefore, be useful to carry out a trial in this area.
As things stand, we would prefer to use Twin Blocks, on most patients with large overjets, presenting in the early adolescence mostly because we are confident that we can achieve our desired result with a functional appliance providing the patient will cooperate with treatment.
Summary
In summary, we feel that the evidence for the treatment of Class II malocclusion is available and can be readily interpreted. This is a mixture of the “art and science’ of orthodontic care. It is essential to remember however that despite being able to improve appearance significantly we just cannot grow mandibles!

Emeritus Professor of Orthodontics, University of Manchester, UK.
what about including oro myofunctional therapy , beginning early in childhood.
The overbit/ overjet discrepancies and malocclusions s are a result of poor maintenance of the growing child and the skeletal deformities causing open mouth breathing / Sleep apnea are to follow.
Should the orthodontist not be involved earlier on in the childs life and be more pro active in th ecranio facial orthopedic growth of the child
No evidence for this at all Dave
And Ive done all the courses in myo.
Not every kid has skeletal discrepancy caused by sleep/breathing issues.
Genetics plays a huge part.
Thank you Kevin for an accurate summary, and guide, based on the evidence for Class II treatments.
I note that no mention is made of the ideal time to treat, as some commentators do, at the period of peak mandibular growth. If all research shows that there is no additional mandibular growth with a two phase approach, and if this is comprehended, then there must be another reason for this belief and practise to persist. I can only think that they believe that the dental changes occur more rapidly at this time. It is surely not ideal to delay treatment for this reason, if a child is being teased or there is a risk of incisal trauma.
Perhaps evidence is not required when you believe you are growing mandibles. Is this still the Flat Earth of orthodontics?
This is an interesting commentary but for a better discussion/understanding, I believe it would be helpful to define the terminology used so we are all on the same starting page. For example:
• What is the definition of a “functional appliance”, as used by the authors in this commentary?
• What is the basis of a “skeletal discrepancy”. Do you mean craniofacial phenotype or something else?
• What is “dento-alveolar compensation”? I believe the authors meant “dento-alveolar Decompensation” (to address developmental compensation similar to our surgical colleagues)
• Who is “we” in the statements ‘we just cannot grow mandibles’? Do you mean orthodontists using evidence-based orthodontic approaches?
References
Kaplan RG. Induced condylar growth in a patient with hemifacial microsomia. Angle Orthod. 1989;59(2):85-90.
Santiago PE, Singh GD, et al. Restitution of the temporomandibular joint in patients with craniofacial microsomia after multiplanar mandibular distraction: Assessment by magnetic resonance imaging. Seminars Orthod. 2001;17(3):186-96
Interesting comment Professor.
I believe the “we”, are those realists who base their opinions on scientific evidence, those blackguards who see the world as it is and not the way you see it. (Apologies to Ambrose Bierce)
We would appreciate your definitions, rather than old references with little scientific merit. That could be the Royal We – or perhaps not!
If I have offended you, then I apologise.
Apologize v. To lay the foundation for a future offence. Ambrose Bierce (1911)
The solution is IMDO, ínter-molar mandibular distraction osteogenesis.
High incidence of numbness
Just for a few weeks and only a partial tingling that fully recovered, at least on my patients.
Russell that is simply not true… there is NO ONE that ever has had numbness from IMDO
Ahh. Thats what I heard anyhow.
Nice to see u watching! Hope u r well Paul 🙂
Russ
And I always thought that IMDO meant, In My Dubious Opinion. I apologise for my igorance
In this same blog Dr. O’Brien recently summarized very accurately that orthodontics cannot improve neither cause or affect OSA patients but what orthodontics can really do with OSA patients is “camouflage” them with all those functional appliances (Herbst, Headgear, twin block, Carriere etc), myofunctional therapy, orthotropics, upper bicuspid extractions to close an overjet, and as we all know all these treatments do not grow mandibles. We also know that “Class II” patients are more prone to perish OSA sooner or later in their lifetime, and as you also said genetics play a huge part.
So if you have a “prominent upper teeth” patient means that has a high risk factor of perishing sooner or later a serious and life-threatening condition and it will be in your hands to decide to “camouflage” his condition so when this patient is 55-60yo would need a big MMA to improve his Apnea/Hypopnea Index having a 10% probability of having a permanent numbness in his lower lip because of the bilateral sagital split osteotomy in order to save him from a serious condition that makes this single patient 7 times more likely to be involved or cause a fatal car accident, 20 times more likely to suffer high blood pressure, 8 times more likely to suffer a stroke or 10 times more likely to suffer a heart attack in their sleep, or either decide to really grow his mandible with IMDO having a probability of 0% of numbness in the long term and save him from the same serious condition.
Totally agree with José Antonio.
IMDO protocol is the right treatment for these kids.
It involves a minor surgery that can be performed from age 12, so it provides an early correction that will have a huge positive impact in the remaining growth (breathing, posture, height…).
IMDO lengthens the mandible, widens the back of it and creates up to 30 mm of arch perimeter.
But if we reduce the overjet earlier… IMDO then is not possible.
IMDO must be an option in these patients… easy surgery, facial improvement, airway improvement, and fantastic occlusal results… for me, no more functionsl appliances….
IMDO must be an option in these patients… easy surgery, facial improvement, airway improvement, and fantastic occlusal results… for me, no more functionsl appliances….results totally different… no stability in many cases, small facial changes, and many tmj problems
No numbness in our patients…. parents super happy with the decission and encouraging other parents to do the same surgery in their children
Affects height? Really? How would you know what height they would have grown to without treatment and if it’s a good thing to affect their height?
I’ve noticed that getting older affects the height of kids. Has anyone else noticed that?
I see lots of Class II patients who are tall and lots who are short and lots in between. I’m not sure how having a Class II malocclusion affects height and how the distractors will know if it’s a tall kid who wants to be shorter or a small kid who wants to be taller or a kid who is just fine with the height they are.
Dear Spencer,
Parents have told me that the posture of their kids changed and their height increased between 1 and 2 cm within the first 14 days of postop, despite the weight loss (inherent to the diet). It’s an increase of height due to a postural correction.
But I must admit that I haven’t measured it. But, even if I had done it, you wouldn’t believe me, am I wrong? 😉
There is also medical knowledge that supports not only these postural changes but an actual increase of growth related to a better oxygenation during sleep.
Best regards,
Sergio
There are too many studies demonstrating that sleep deprivation, OSA in pediatric patients cause less secretion of Growth hormone at night, and when the problem is solved the growth hormone release becomes normal again.
Some cites just to name a few:
1. Effects of Sleep and Sleep Deprivation on Interleukin-6, Growth Hormone, Cortisol, and Melatonin Levels in Humans, The Journal of Clinical Endocrinology & Metabolism, Volume 85, Issue 10, 1 October 2000, Pages 3597–3603,
2. Sassin, J. F., Parker, D. C., Johnson, L. C., Rossman, L. G., Mace, J. W., & Gotlin, R. W. (1969). Effects of slow wave sleep deprivation on human growth hormone release in sleep: preliminary study. Life Sciences, 8(23), 1299-1307.
3. Brandenberger, G., Gronfier, C., Chapotot, F., Simon, C., & Piquard, F. (2000). Effect of sleep deprivation on overall 24 h growth-hormone secretion. The Lancet, 356(9239), 1408.