Do orthodontic retainers and extractions reduce marginal bone levels?
Do orthodontic retainers and extractions reduce marginal bone levels?
This post is about a new study that investigates the effect of retainers and extractions on marginal bone levels. I thought it was very interesting as it included an evaluation of the effect of extractions.
Some of my most popular posts have been on methods of orthodontic retention. I have pointed out that there is not a high level of evidence to help us decide on the type of retainers that we use. Nevertheless, we do appear to know that even though retainers may encourage plaque accumulation, this does not seem to translate into periodontal disease. I was very interested to see this new study that a team from Gothenburg in Sweden published in the AJO-DDO.
Anna Westerland et al.
Am J Orthod Dentofacial Orthop 2017;151:74-81.
DOI: http://dx.doi.org/10.1016/j.ajodo.2016.06.029
They did this study to find out if bonded orthodontic retainers had any adverse effects on the marginal bone levels of the lower incisors.
I thought the literature review was very good. They pointed out that we have limited knowledge on the possible adverse effects bonded retainers on oral health. They also questioned whether the fixing of teeth together was harmful to periodontal health. Finally, they suggested that previous research has been somewhat limited because the main outcome measure was marginal bone height recorded from two-dimensional radiographs.
The authors did this study to find out if bonded orthodontic retainers had any adverse effects on the marginal bone levels of the lower incisors using Cone Beam Computed Tomography.
What did they do?
They studied patients who had finished treatment between 1998 and 2002. They included patients treated with fixed appliances who had complete pre and post-treatment data, study models, and profile radiographs.
The investigators recalled the patients, at least ten years after they completed their orthodontic treatment, and measured their marginal bone levels using CBCT. The study also had a retrospective component because they looked back at possible predictive variables on the bone levels.
They divided the patients up into three groups
- Multi strand lingual retainers bonded from canine to canine
- No retention
- A control group of untreated people.
The marginal bone level, recorded by CBCT, was the primary outcome.
They selected several predictive pre-treatment variables. These were; the presence of a retainer, incisor irregularity, incisor angulation, selected cephalometric variables and whether the patients had had extractions.
They carried out appropriate complex statistics.
What did they find?
They found statistically significant differences in marginal bone levels between the groups. Importantly, the marginal below levels were lower for both the retained and no retention groups compared with the control. However, there was no difference between the retainer and no retention groups. I have put some of the data in this table.
| Pre-treatment | Post-treatment | |
|---|---|---|
| A-P condylar position | 5.77 (4.47-7.06) | 6.82 (5.42-8.22) |
| Anterior joint space | 3.1 (2.39-3.81) | 3.9 (3.12-4.68) |
| Posterior joint space | 2.78 (2.4-3.09) | 2.23 (1.96-2.5) |
They also showed that reduced bone levels were associated with a posterior rotation of the mandible, long face growth traits, extractions, incisor retroclination and high irregularity index at the start of treatment.
They concluded:
‘Long term retention in general does not seem to cause any adverse effects on the marginal bone levels 10 years after orthodontic treatment”.
What did I think?
This study may provide us with useful information. However, before I interpret the results, we need to bear in mind the type of study design they adopted. It is important to consider that this is a retrospective study. As a result, it has selection bias. For example, they only selected patients with complete records. We do not know about the patients whose records were incomplete. Secondly, it was cross-sectional. This means that we do not know anything about the marginal bone levels at the start at the end of orthodontic treatment.
The authors have pointed out these problems with their study in their nicely written discussion. Nevertheless, the results are very interesting. Importantly, the fixed retainers did not cause harm. This is consistent with other research findings and we are beginning to build a clearer picture on this clinical issue.
However, the big “headline grabbing” finding was that extraction and retroclination of the lower incisors were associated with bone loss. But before we all get too excited about this data, it is important to consider that pre-treatment irregularity was also associated with bone loss. There is a possibility that this may have led to the thinning of the alveolar bone.
We also need to consider the effect size and whether this is clinically significant. For the buccal surfaces of the incisors the bone loss was 1.7 mm. I’m not sure whether this is clinically significant and it is up to individual operators to decide on this for themselves.
Nevertheless, I do feel that these findings are very interesting and certainly deserve to be studied in a long-term prospective study.
Does this change my practice?
Finally, does the study change my practice? I feel that this is a small study that is subject to selection bias and has a high level of uncertainty. As a result, it will not change my practice but it will certainly make me think.
I think that there will now be a lively discussion about this findings in the comments page of this blog.

Emeritus Professor of Orthodontics, University of Manchester, UK.
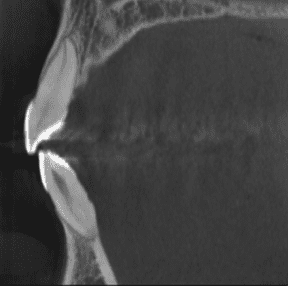 Cone-beam computed tomographic evaluation of the long-term effects of orthodontic retainers on marginal bone levels
Cone-beam computed tomographic evaluation of the long-term effects of orthodontic retainers on marginal bone levels
I would assume that for a periodontist a loss of 1.7 mm of buccal bone may be clinically relevant. Because of the wide confidence interval the difference can be seen as high as around 3 mm (visual “statistics”). Controlling somehow for OH would have been nice. Too bad that Figure 3A is not clinician/reader friendly. It would have been nice to have some idea of the strength of the association with extractions and retroclination of incisors. Maybe is simply may lack of understaning of the presented table and the information is there. How much were those two related with the magnitude of discrepancy to start with? Finally, as mentioned without knowing where the bone leves where it is challenging to further interpret the findings.
I don’t understand why age of the patients in group 1,2 and 3 is not discussed in the abstract.
For me as a clinician is obvious that bone level of a patients (10 years after treatment and control) depends much on the age and also on the level of oral hygiene.
Thank you for your effort. I think this study doesn’t change my work. I think this study could help me to evaluate which type of retention use for my patients.
Roberto
After 36 years of active practice, I look back at who were my mentors. One of my primary mentors was Bjorn Zachrisson. I basically did everything he suggested. I varied little from his recommendations. I figured that he had it figured out and why do I need to reinvent the wheel. He recommended fixed retainers and I took to the idea wholeheartedly. Now after almost a lifetime in practice, I have mothers bringing in their sons and daughters. They ask me if I remember them because I did their orthodontic treatment years previously. I always ask to look at their smiles and it makes me feel pretty good about how nice things look and I think it goes without saying that they are back because of the persistence of their orthodontic result. Most of them are still wearing a fixed lower retainer bonded just to the canines as recommended by Dr. Z. I practice in a working class area and it makes me feel their parents money was well spent.
In the article referenced by Dr. O, the fixed lower retainer was bonded to all teeth so I have to assume that one bonded just to the canines would have done at least as well and probably better. There is just no comparison between fixed retention just to the 3’s and removable lower retainers. If you are able to achieve normal OB/OJ at the end of active tx, the lower retainer tends to hold the entire system together on a long term basis.
When patients ask me when they can have their fixed retainer off, I tell them to contact the office when they start looking at nursing homes brochures. 🙂